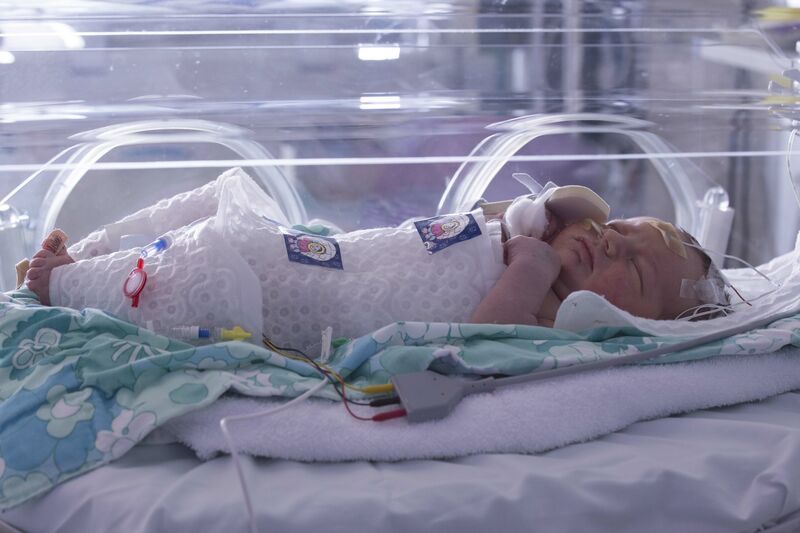
Hypoxic-ischaemic encephalopathy (HIE) may be diagnosed if your baby’s brain does not receive enough oxygen and/or blood flow around the time of birth.
- ‘Hypoxic’ means not enough oxygen
- ‘Ischemic’ means not enough blood flow
- ‘Encephalopathy’ means it is affecting the brain.
You might also hear it being referred to as ‘asphyxia’, ‘birth asphyxia’ or ‘perinatal asphyxia’.
Low oxygen and/or blood flow to a baby’s brain happens most often before or during birth, but it can also happen shortly after birth.
HIE affects the brain, but low oxygen or blood flow can also cause problems in the lungs, liver, heart, bowel and kidneys.
When diagnosed, HIE is graded as mild (stage 1), moderate (stage 2) or severe (stage 3). Where HIE is graded as moderate or severe, it can result in long-term disability and in some cases can sadly result in death. We have more information about making critical care decisions, palliative care and bereavement, and links to other sources of support further down this page.
If your baby has been diagnosed with HIE, you are likely to have lots of questions about what caused this, what treatment your baby will need and how the condition may affect them in the long term. Talk to the staff looking after your baby. They will be able to answer your questions and explain what is happening.
What causes HIE?
It is not always possible to know what causes HIE. It can be caused by complications during pregnancy such as:
- Issues with blood flow to the placenta
- If the birthing parent suffers from high blood pressure
- Issues with the baby’s lungs
- If the birthing parent suffers from alcohol or substance disorder
And it can be caused by complications at or around the time of birth such as:
- The placenta coming away from the uterus wall too soon (placental abruption)
- Tearing of the uterus (uterine rupture)
- Having an unusually long labour (prolonged labour)
- Your baby’s shoulders getting stuck behind the pubic bone during delivery (shoulder dystocia)
- Cord entanglement or compression, where the umbilical cord is unable to function correctly.
HIE can occur at any stage during a pregnancy, during labour or shortly after birth. During labour, the medical team will be monitoring your baby’s breathing and heart rate. After delivery, Apgar scores (a general well-being check on new-born babies) may indicate early concerns.
HIE is usually diagnosed in the first few days after birth. A doctor will make the diagnosis based on certain signs, which are different depending on how severe the condition is.
What are the signs of HIE?
Doctors will look for some of the following signs in your baby:
- Being hyper-alert – they may appear over-awake, even with little sleep
- A reduced level of awareness or responsiveness or being overly sleepy
- Being irritable – they may start to dislike noise, touch and light
- Having unusual movements or seizures
- Having pauses in breathing (apnoea)
When diagnosed, HIE is sometimes referred to by the Sarnat Scale as Stage 1 (mild), 2 (moderate) or 3 (severe). The grade of HIE will determine the treatment that is recommended for your baby.
What tests might my baby have?
If your baby's healthcare team is concerned about the possibility of HIE, they may arrange further tests. These might include (but are not limited to) the following:
- Cerebral Function Monitoring (CFM) – CFM uses sensors to record brain activity. It is used to show the early effects of HIE on your baby’s brain, and can be also used to decide if your baby needs therapeutic hypothermia (cooling) treatment.
- Head ultrasound scan (cranial ultrasound) – A head ultrasound scan is used to look at images of your baby’s brain. It can be used to show problems such as bleeding, stroke or swelling.
- Checking cord blood gas levels – A buildup of acid in the umbilical cord artery may indicate there is a risk of damage to the brain.
- MRI scan – An MRI scan uses magnetism to build up a very detailed picture of areas of your baby’s brain. It is used to see if any damage has been done to your baby’s brain. It is usually performed after cooling treatment (see below).
Treatment for HIE varies depending on how severe it is believed to be.
Mild HIE (Stage 1)
Most babies with mild HIE recover quickly. If your baby has mild HIE, doctors will monitor them closely to check that they are stable and ensure they do not need any more treatment.
Should your baby need additional support, they may be referred to one or more Allied Health Professionals (AHPs) to provide support and advice during your baby's inpatient journey and, if needed, continue to provide early intervention support on discharge. Allied Health Professionals include services such as physiotherapists, occupational therapists, dieticians and speech and language specialists.
Moderate to severe HIE (Stages 2 and 3)
If your baby has moderate to severe HIE, there is a risk of long-lasting damage to the brain, or death.
To reduce this risk, babies with moderate or severe HIE are likely to receive a treatment called therapeutic hypothermia or cooling therapy, which needs to be started within the first 6 hours after birth. A special cooling mattress is used to lower the baby’s temperature to between 33°C and 34°C for 72 hours. The mattress is filled with fluid that can be cooled or warmed according to your baby’s needs. This helps to slow damage to brain cells and prevent further toxins from forming, limiting injury to the brain.
Your baby’s temperature will be monitored closely to ensure that it stays at the right level, and cooling will usually be continued for 72 hours before rewarming. Your baby will be rewarmed over a period of 12 hours. During the cooling period, the team will also closely monitor your baby’s heart rate and blood pressure, perform blood tests and use a Cerebral Function Monitor (CFM) to record brain activity. They will also monitor your baby’s medication and give pain relief and anti-seizure medication if needed.
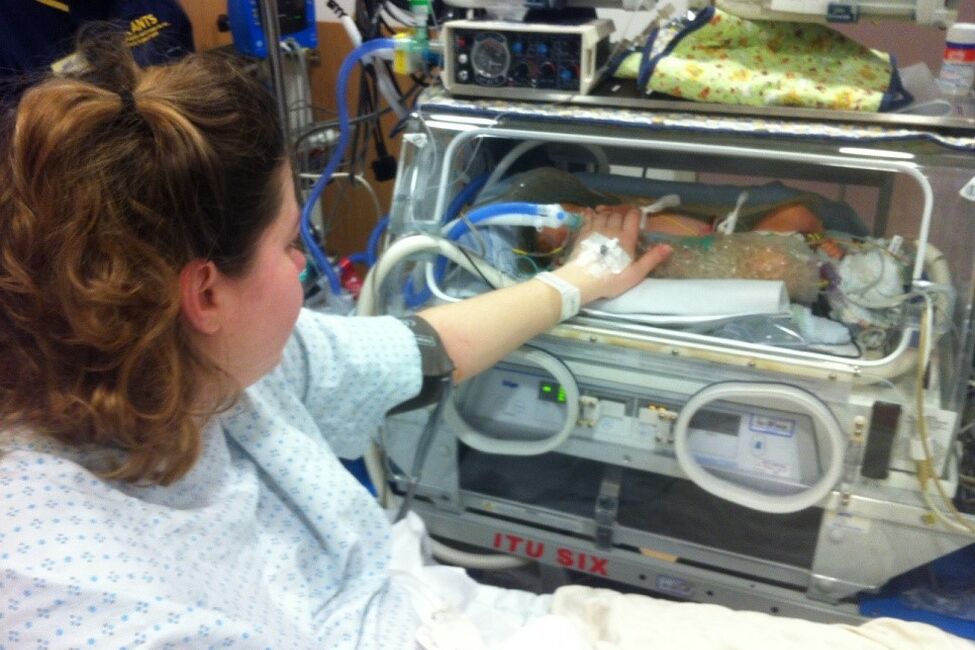
Some parents are worried that they will not be able to hold or have skin-to-skin with their baby during cooling treatment. You may be able to hold or touch your baby during cooling, but this depends on how unwell your baby is and how much equipment is attached to them. Talk to your baby’s neonatal team to understand how you can be involved.
During this time, you can also help your baby by expressing breastmilk and talking and reading to them.