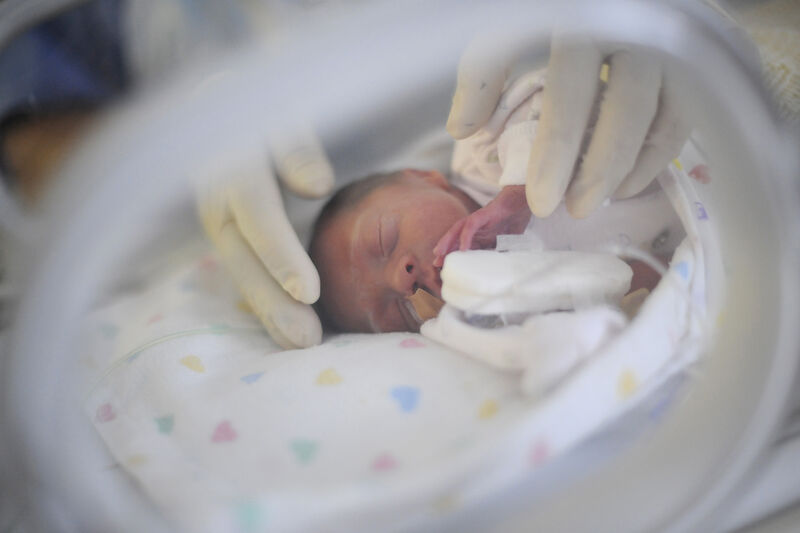
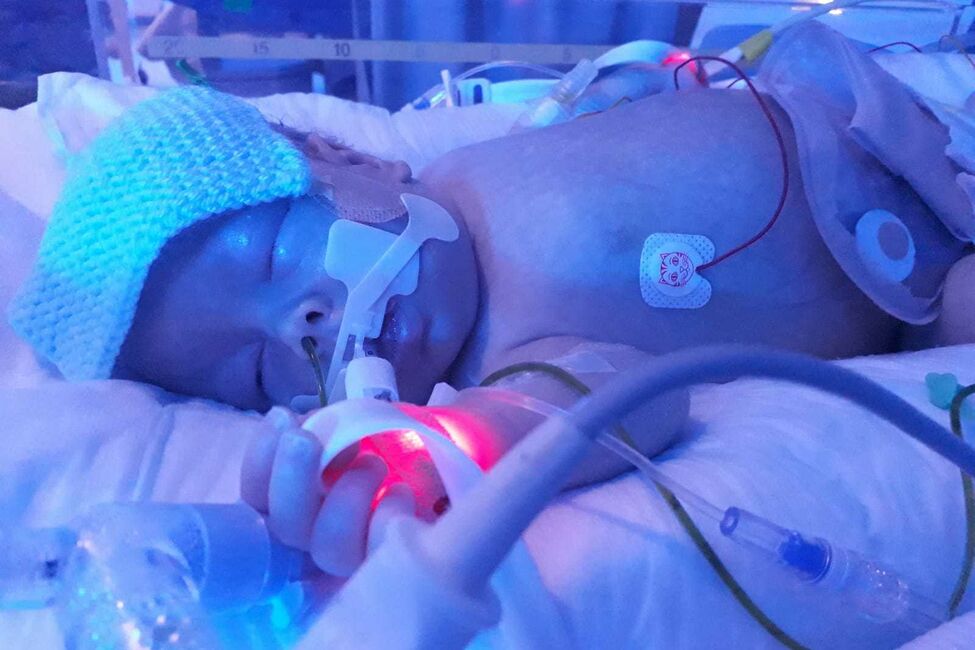
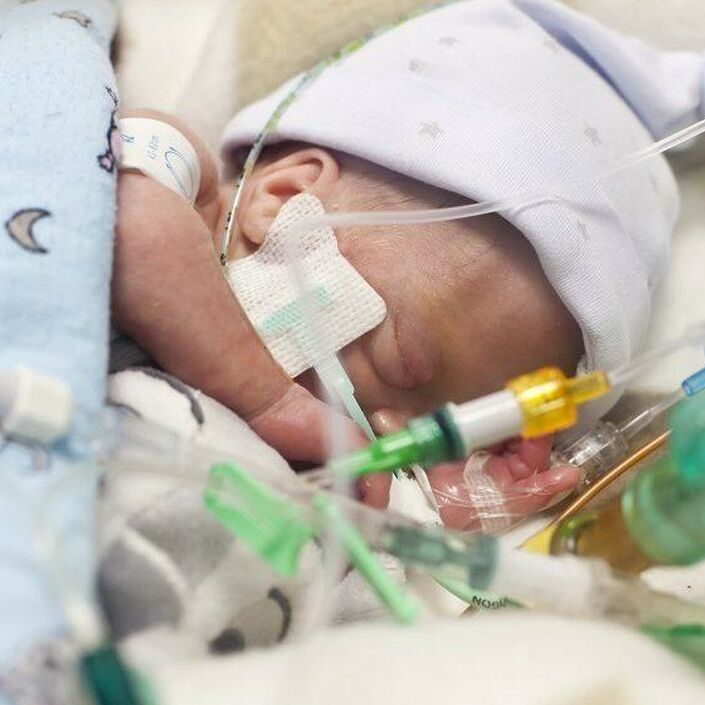
Necrotising enterocolitis (NEC) – a serious condition that mainly affects babies that are born premature – is where tissue in the bowel (small and large intestines) becomes inflamed. Doctors may describe NEC as an inflammation of the gut. NEC can affect just a small part of the bowel, multiple parts of the bowel, or sometimes the whole bowel can be affected.
How serious is NEC?
NEC is a serious condition and babies can become very unwell. NEC can settle with medical treatment, but sometimes tissue in parts of the bowel will become more damaged and will need to be removed with surgery.
Sadly, some babies will die as a result of NEC. They may be too unwell for surgery or they may not get better with treatment. You should always be given the opportunity to discuss your baby's care and treatment with your neonatal team. This team might include neonatologists, occupational therapists, neonatal nurses and dieticians.
We know that having a baby with NEC or suspected NEC might be frightening. The staff on the neonatal unit are there to support you and can answer any questions you may have.
We have more information about making critical care decisions, palliative care and bereavement.
Doctors do not fully understand what causes NEC. It is a complex condition and there are likely to be lots of possible factors.
It is clear that it mainly occurs in babies born premature (at less than 37 weeks of pregnancy) or sick. They have immature bowels, which means they are more likely to develop NEC than a baby born at full term (37+ weeks of pregnancy).
Who is most likely to get NEC?
NEC usually affects newborn babies in the first few weeks after birth. It is more common in:
- premature babies (particularly babies born before 32 weeks or who weigh less than 1500g)
- babies who have complex medical problems, such as congenital heart defects
- babies who have been unwell before they were born (for example, babies who are not growing in the womb as expected).
NEC is most likely to affect babies before they go home from the neonatal unit. NEC can also affect babies born at term and who have been otherwise well, although this is rare.
NEC is difficult to diagnose. Some of the symptoms of NEC are general signs of being unwell or fighting an infection such as:
- a fast heart rate
- low blood pressure
- irregular, fast, or slow and shallow breathing
- a high, low or quickly changing temperature.
In some cases, more specific signs indicating NEC may develop, which may include:
- not feeding as usual
- blood in their stools (poo)
- a painful, swollen or discoloured tummy
- being sick (vomiting), especially if they are vomiting green liquid (bile)
- having a large volume of green fluid, or blood coming back up your baby’s NG (nasogastric) tube (if they are being fed by a tube).
What tests might my baby have?
It can be hard to know if these symptoms are caused by NEC or another condition. If doctors suspect it might be NEC, they will perform some tests, which may include:
Sometimes they may also do other tests, such as an ultrasound or faecal tests (where they test poo for traces of blood). Even with the results of these tests, it’s still difficult to be certain of NEC and treatment may begin before a diagnosis has been confirmed.
Always speak to a healthcare professional if your baby is not their usual self, or if you think your baby is becoming unwell. Parents know their baby best and may be able to spot signs of discomfort or illness before they become obvious to a healthcare professional.
If you think your baby is seriously unwell, alert staff on the neonatal unit or call 999 if you are at home. Things can change very quickly and your baby may need additional medical care or transfer to another unit with specialist surgical care.
Research shows that babies fed with breast milk are less likely to develop NEC, however, babies who have only been fed breast milk can still get NEC, so this does not completely remove the risk.
Babies born premature may be unable to breastfeed in the first few weeks. If this happens, you can help protect your baby by starting to express your milk. This is then fed to them through a tube into their tummy. By doing this, your baby can still get the benefits of having your breast milk.
If your baby cannot take milk at this time but you want to feed your baby breast milk later on (either by breastfeeding or bottle feeding), you should continue to express breast milk.
Using breast milk may also be helpful when your baby is recovering from NEC and is able to start milk feeds again. If you are finding it difficult to express breast milk, some neonatal units may have access to donor milk. Talk to staff at your unit for more information.
Healthcare professionals will be able to help you with feeding your baby. You can also visit our pages on feeding for more information.
If your baby has mild NEC, or healthcare professionals looking after your baby think your baby may have NEC, the following treatments may be started:
Inserting a gastric tube
A tube will be inserted into your baby’s nose or mouth to remove air and fluid from their stomach.
Stopping milk feeds
This allows the bowel to rest, which can help it recover. When milk feeds cannot be given, your baby may be given nutrition, such as fat, sugar, protein and vitamins, through total parenteral nutrition or TPN.
For this, a soft plastic tube called a long line or PICC (peripherally inserted central catheter) is inserted into a vein in your baby’s arm or leg allowing them to be fed all the nutrients they need directly into their bloodstream. This is to make sure your baby grows while they are not being fed milk.
Starting antibiotics
Antibiotics will be given to treat and prevent infections through the long line. They may be given for up to 14 days.
Support with breathing
If your baby needs help with breathing, they will be put on additional oxygen. This could mean:
- they have a tube in their nose, which is connected to an oxygen supply
- they wear a small CPAP mask, which gives continuous positive airway pressure to support the lungs
- they are placed in a ventilator to help inflate your baby’s lungs.
Many babies who have NEC start to respond to these treatments within 72 hours (3 days) and regular feeding might be reintroduced after 14 days. However, babies will need surgery if:
- they do not respond to treatment or the condition worsens
- there is a hole (perforation) in the bowel
- part of the bowel dies.
We have more information about surgery to treat NEC.
Your baby’s medical team should keep you aware of your baby’s care at all times, and you should be able to make decisions with them about your baby’s care. See our guidance on working with healthcare professionals for some of the questions you could ask and what procedures you can be involved in, if you wish to be.
What might happen after treatment for NEC?
Many babies recover well from NEC, but it is possible that other problems may develop including:
- NEC coming back (recurrent NEC). If this happens, your baby may need surgery. We have more information about surgery to treat NEC.
- Strictures, which is where the bowel narrows because of scar tissue. This can be caused by damage to the bowel from NEC, or from surgery to treat NEC. If this happens, surgery will be needed to widen the area of bowel or possibly remove the narrow area.
Your baby may need surgery if any problems continue.
In the long term, some research shows that NEC can have an impact on how some babies’ brains develop, but it’s important to remember that all babies develop at different rates. Your baby’s development will be regularly assessed and monitored by healthcare professionals.