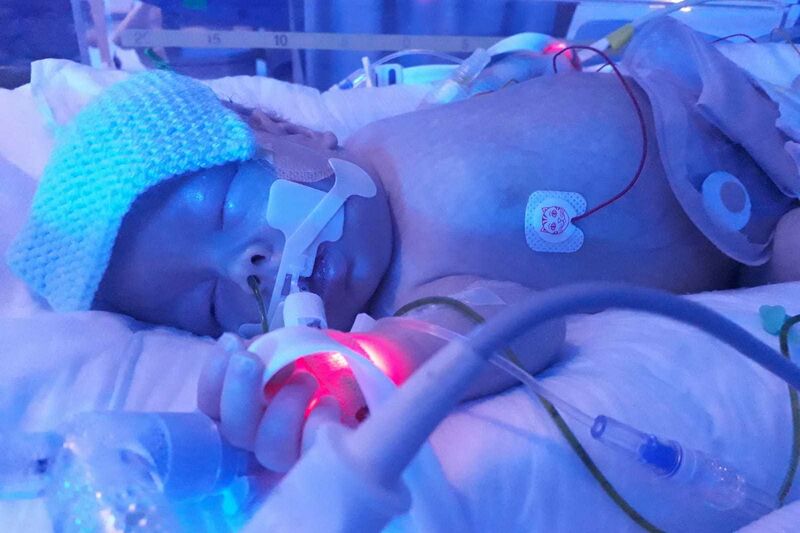
Kane had necrotising enterocolitis (NEC). They told us he was extremely poorly and that they were going to use three different antibiotics to treat him but if these didn’t work they’d have to perform surgery. Even seeing how ill he was, I never thought it would get to that and was sure the drugs would do the trick.
We stayed with Kane until the early hours of the morning. We had been given a parent room on the unit and a nurse sent us to try and get some sleep.
There was a knock on our door at around 6.00am. The doctors were now struggling to ventilate Kane. His stomach had become so swollen that there was no longer enough room for his lungs to inflate.
I walked into intensive care and a surgeon was in there talking on the phone.
She said: “I’ve got an extremely poorly baby. Prepare the theatre; I’m bringing him over now.”
It took me a minute to realise the baby she was talking about was my own.
I was handed consent forms and told all the risks of the surgery – including death. This terrified me but she also said that if they didn’t take him for the surgery now, he wouldn’t have any chance of survival at all. We had to give him that chance. No words can explain my heartache and pure terror as I signed that consent form.
Kane’s dad and I walked our baby to the theatre. I kissed Kane’s head and told him that he could do this. I told him how amazing I thought he was and that I could never explain how proud of him I was or how much I loved him.
We were taken back to our bedroom and were told that someone would come and get us as soon as there was any news.
We just sat there, staring into space and fearing the worst. I didn’t know if I’d ever see my baby again and I was terrified.
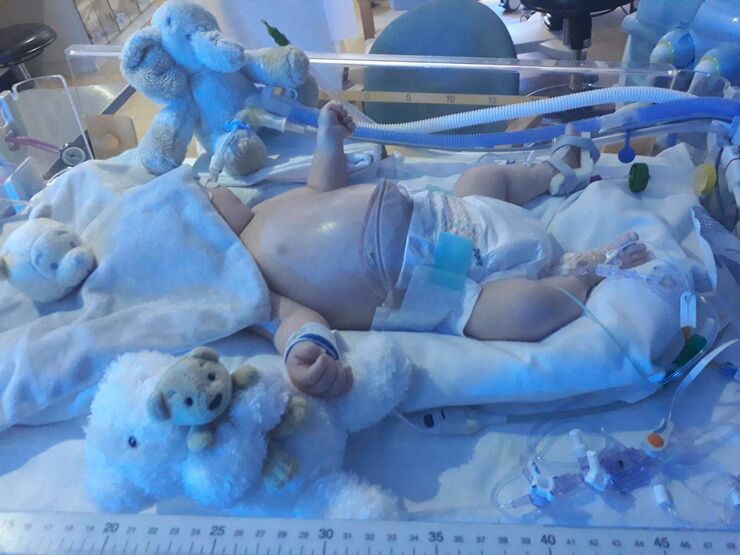
After around 90 minutes, the surgeon knocked on the door. They’d removed a small part of Kane’s bowel, drained fluid from his abdomen and formed a stoma to give the infected part of his bowel a rest. The operation had gone to plan but we’d have to see how he responded in the next few days.
When we went to see him, Kane was on another kind of life support that was causing him to vibrate as several breaths per second were delivered. As he lay there sedated with a stoma, I had no idea how I was going to care for him and felt terrified of hurting him if I touched him.
We had Kane christened as soon as he was stable, a couple hours after he returned from theatre. They put screens up around his crib and the hospital chaplain performed the service. It was not the christening service you expect to have; usually the service is a joyous day full of fun and surrounded by friends and family. We weren’t sure at that point which way things were going to go and it was important to us that it was done in case the worst was to happen.
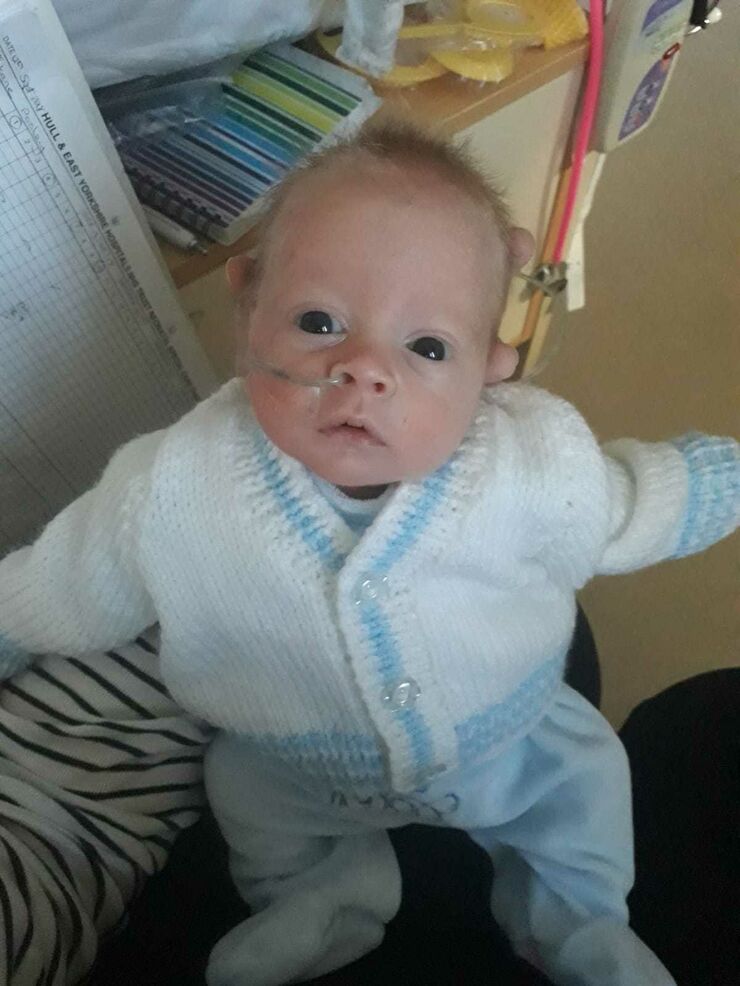
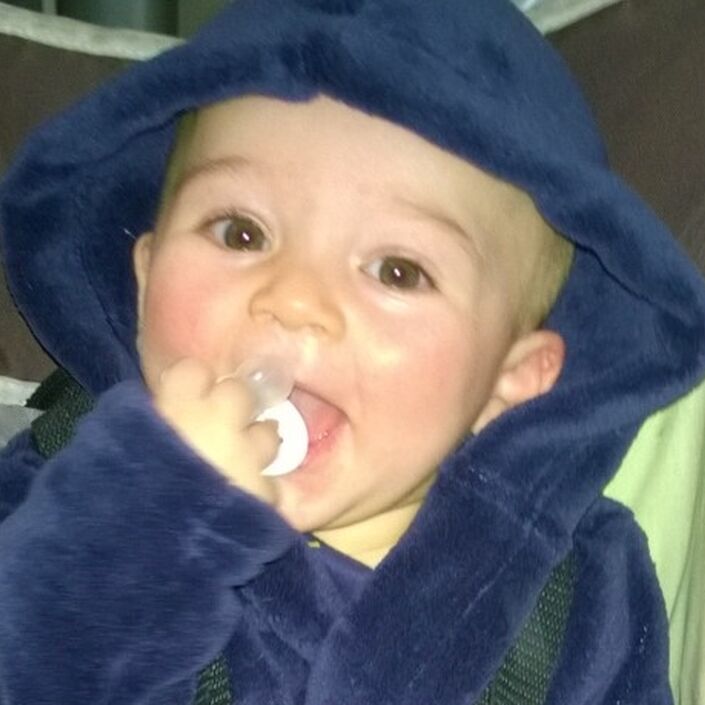
Nothing changed for a gruelling six days. Then on day seven, the surgeon told us Kane was starting to show signs of improvement. The relief that coursed through my veins was unbelievable.