Many parents find comfort in expressing as it is something positive and important they can do for their baby. Try not to compare the amount you are expressing with others, as they may have faced different challenges or situations to you.
Expressing breast milk can also take time to learn. The staff looking after your baby will give you support and practical help with this. Speak to your neonatal nurse, feeding specialist or midwife for more support.
In this section, we have more specific information about:
If you have any questions about expressing or are not sure what to do, you should always ask questions or seek more support. Most units will provide specific support with expressing, and your neonatal nurse will be happy to help with any questions that you have.
How often should I be expressing milk for my baby?
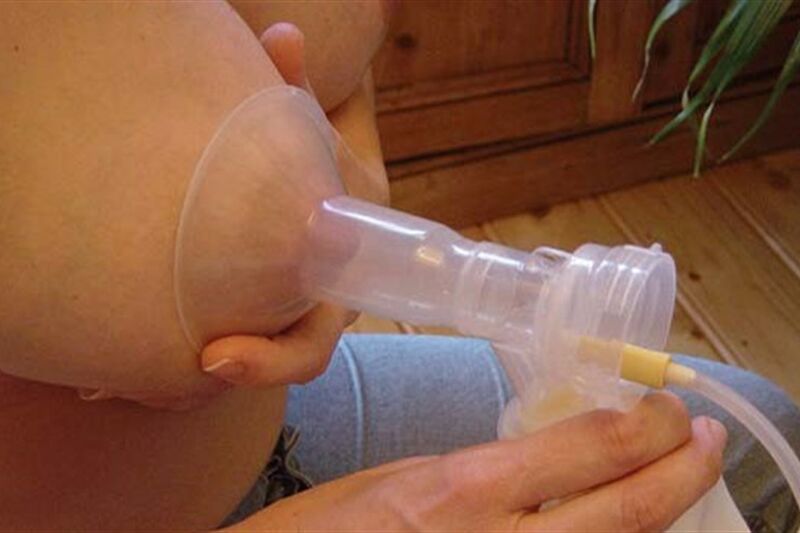
It is important to start expressing milk as soon as possible after your baby is born – ideally within two hours. It is recommended you express frequently to keep your milk supply up. To begin with, this is around eight to ten times in 24 hours, including at least once at night. This is because breast milk is produced on a demand and supply system, so you are likely to produce less milk overall if long periods of time are left between expressing.
In time you will find what works best for you. You may find that your milk flow responds to a fixed routine and will trigger a let-down reflex (see below), which will make it easier to express. This might include actions when you prepare to express, such as removing equipment from the steriliser, or putting the pump together.
The let-down reflex
When you express milk, you may notice tingling or prickling in your breasts and nipples, or a feeling as if the milk is rushing in to fill them. This is called the let-down reflex (it is sometimes called the milk ejection reflex). During the let-down reflex, a hormone called oxytocin is released, which helps with milk flow. This takes a few minutes to appear at first, but later it will happen in a few seconds.
The let-down reflex feels different to different women. Some mothers describe a slight pain and some mothers have no sensations at all. Your body may respond to certain things you do, which can trigger your let-down reflex. For example, it is normal for the let-down reflex to happen in response to having a warm bath or shower, or to breast massage (see below). It can also happen in response to being close to your baby, hearing your baby cry or having a picture or something close by that smells of them.
Staying as relaxed as possible and having skin-to-skin contact with your baby can all help to trigger the let-down reflex. Taking some deep breaths and concentrating on your breathing can help with this. It will also help to express at your baby’s cotside if this is possible, so you can be close to your baby. Speak to the staff looking after your baby about this.
Gentle breast massage
Breast massage before expressing can help to trigger the let-down reflex and stimulate your milk flow. You can do this by gently stroking, rolling, kneading, and tapping your breasts with warm hands before hand expressing and/or using a breast pump. You should do this for at least two minutes. Breast massage during expressing can help to drain your breasts.
Looking after yourself when expressing
Expressing milk for your baby can be a great way for parents to feel more empowered and in control of their baby’s care. Many mothers also tell us how difficult and exhausting it can be to express, especially at night. This can be a particularly difficult experience if their baby is not with them.
It can be a very stressful time, but it is important that you try to stay as relaxed as possible when expressing, as this helps with the let-down reflex and milk flow. Some research has shown that higher stress levels may contribute to the delay of milk production. Some parents find that having a photograph or something that smells of their baby nearby when expressing helps. It may also help to distract yourself by doing something like reading a book or watching TV when you express. Listening to soothing music, meditation or taking time to focus on your breathing may also help you to relax.
Partners can help with expressing. For example, they can offer encouragement, help you to relax, or get equipment ready.
It is not unusual to find feeding your baby a difficult experience. In our survey of over 100 parents, over 60% said that their mental health got slightly or significantly worse during the experience of feeding their premature or sick baby. It is okay to find the experience difficult, no matter your situation. Every parent will have a very different experience of neonatal care.
It is important to talk to someone if feeding your baby is having an impact on your mental health. This could come from your feeding specialist, neonatal nurse, midwife, doctor, partner, or friends and family. We have lots of information about the impact having a premature or sick baby can have on your mental health, and where you can get support.