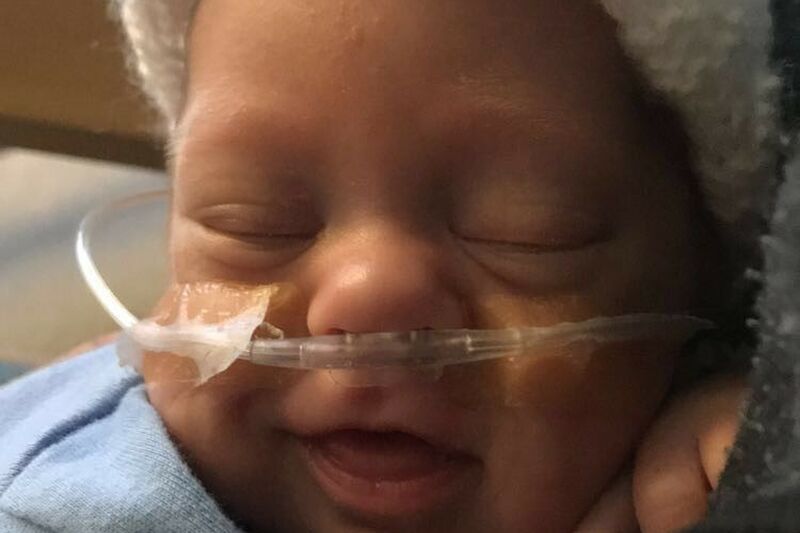
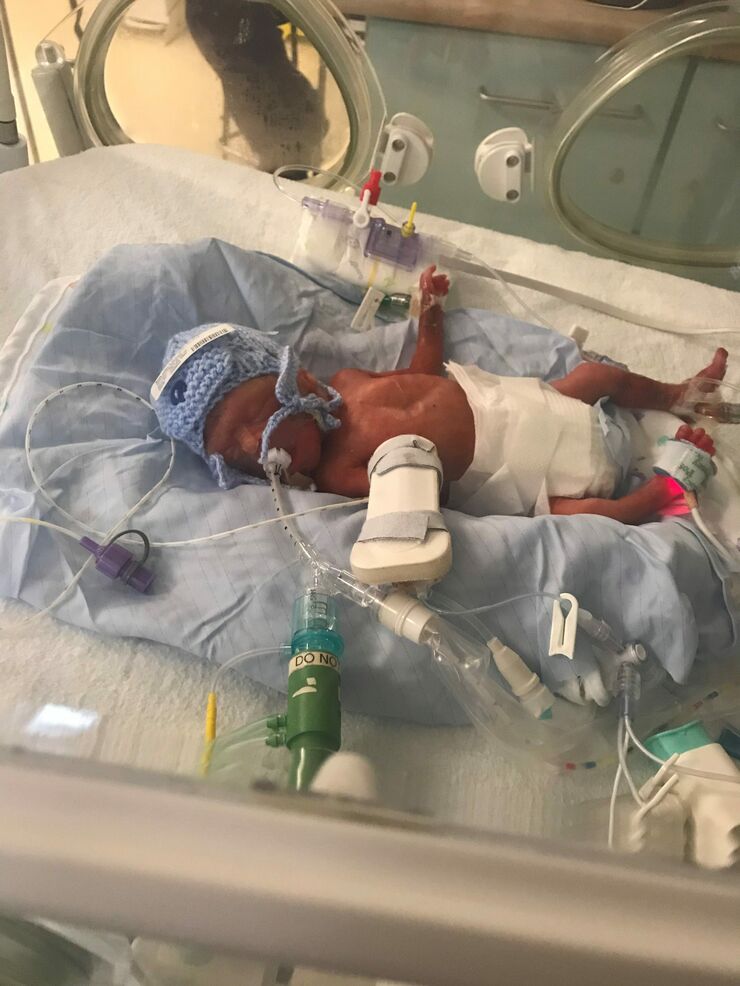
Eight years ago, I had my beautiful daughter Bonnie at full term. After having Bonnie, I decided to go on the copper coil but a few years later had the same feelings of morning sickness I did when I was pregnant with her.
Unlike the Mirena coil, when you are on the copper coil, you still have your periods. When my next one was late, I took a pregnancy test. It was positive. I was in total shock and although the baby was not planned, a part of me felt like it was meant to be.
I didn’t know anyone who had fallen pregnant while on an IUD so asked my doctor how the coil would affect the pregnancy. The GP was unsure and so I was booked in for a scan at seven weeks which revealed a heartbeat. The sonographer couldn’t see the coil and so it was assumed that it had fallen out. I was told to return to the hospital for my 12 week scan.
At nine weeks, I had the first episode of heavy bleeding. Initially I thought I had a miscarriage and rushed to the hospital. By the time I reached the waiting area, I had lost so much blood that I passed out. When I came round, I was lying in a bed in the ward, attached to a drip with my worried partner sitting next to me.
I was given an abdominal scan and this time the IUD was spotted just above the foetus in my uterus. The doctors told me that they would not be able to remove the coil as its positioning would cause a miscarriage. I was advised to do minimal activity because my chances of miscarrying were 50 per cent higher than other women because of the presence of the coil. This news was absolutely terrifying.
The episodes of heavy bleeding returned at 11, 15 and 17 weeks. Each time I rushed to hospital thinking the worst but then was reassured things were ok. It was horrible – I was in tears every single time.
At 20 weeks, my scan showed the baby was growing well and was a good weight. Shortly after the scan, I began to bleed every day and was admitted to hospital. I felt totally exhausted, missed my family and was so worried about the baby.
Whilst staying at the hospital, a consultant revealed that the scan had also shown that there was a massive blood clot above the sac – right where the coil was. He said that it was likely that I was going to have a late miscarriage and it would probably be within a matter of weeks. I refused to believe it. We had come so far - I prayed that I could keep this baby safe.