I was prepped for a C-section and went into the operating theatre with my mother-in-law. I wasn’t feeling to great, due to the stress and worry, so we decided she would come in with me, as she is just like a mum to me.
I was laid on the bed with my waters were broken, and then there was mass panic. The midwife was shouting, the doctor was holding onto my baby's head from inside, whilst there was lots of gushing. The anesthetist and his assistant were telling me "goodnight mum" (code word for "you need to be put to sleep for an emergency C-section", which was discussed before we went in).
As the room filled with people, all I could do was sob with a mask over my face (which I had to wear because of COVID 19), having my tummy prepped for surgery and thinking "please hurry and get my baby out".
My daughter, Evie, was born at 2:45pm and had to be resuscitated, as she had been without oxygen for 11 minutes and lost a lot of blood.
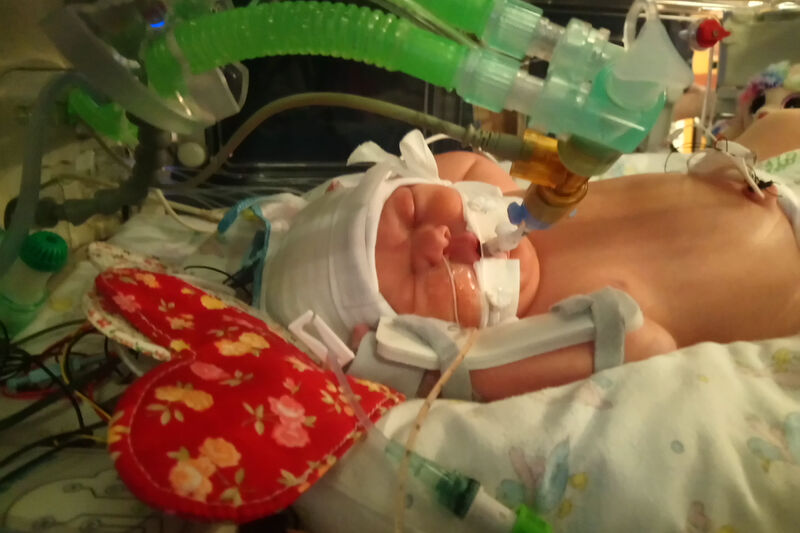
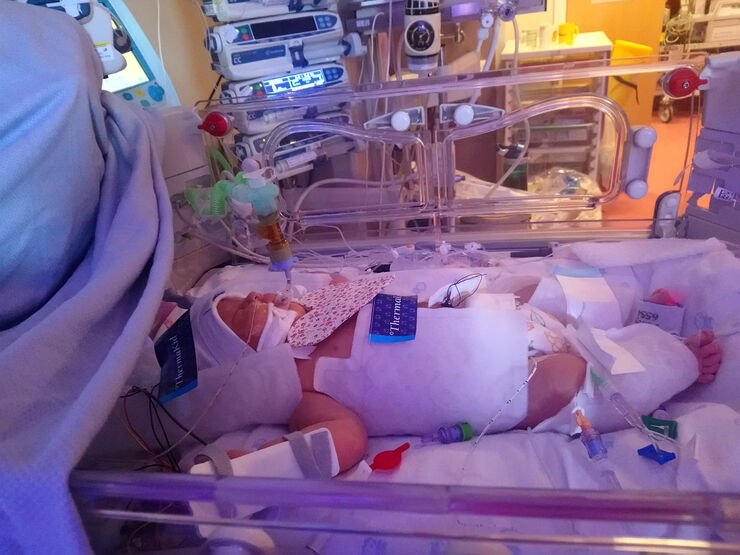
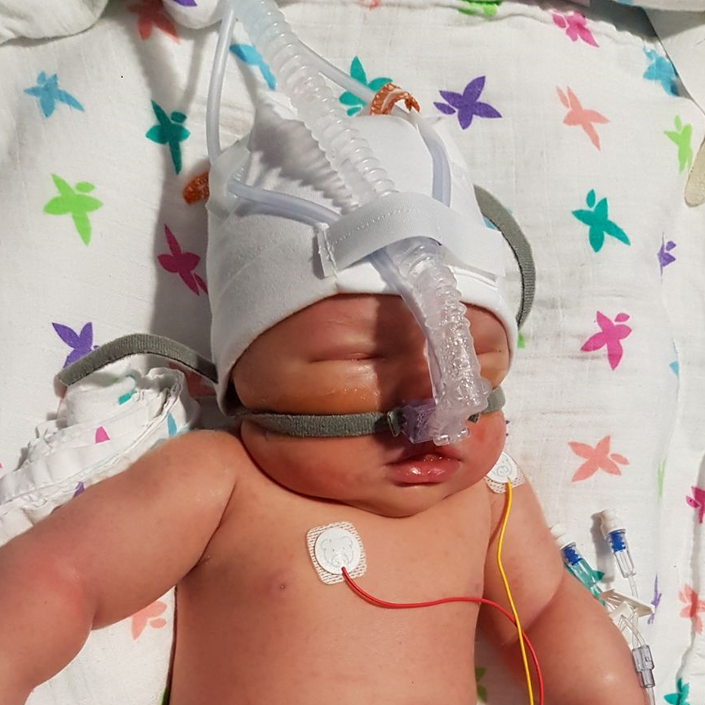
The next ting I knew, I was in recovery, feeling very groggy, and being monitored for hours. I was finally taken to a room on delivery suite and told my baby was very poorly. I was told she had suffered HIE and that dad was with her, and would take a picture for me.
They explained that she was being transferred to another hospital for cooling treatment, as my hospital didn’t have it. Sadly I couldn’t go, as I had pre-eclampsia and had to stay on a magnesium drip for 12 hours. My blood pressure went up to 200/110 and I had lost a lot of blood.