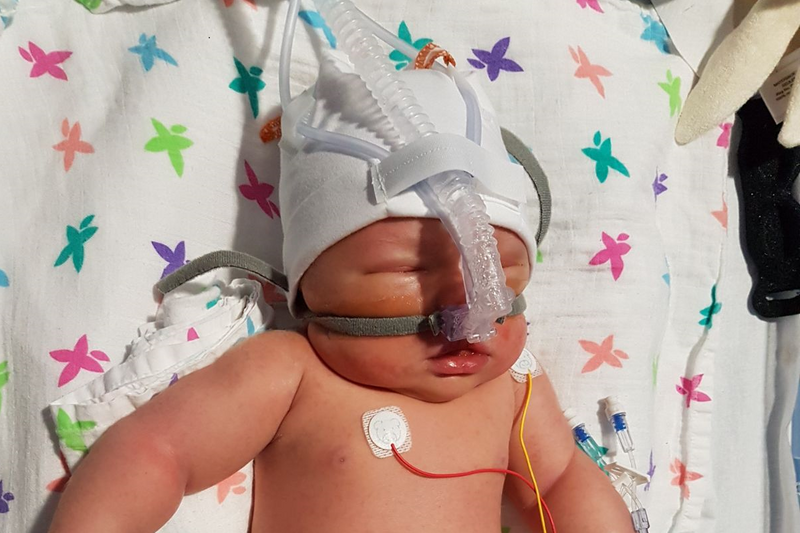
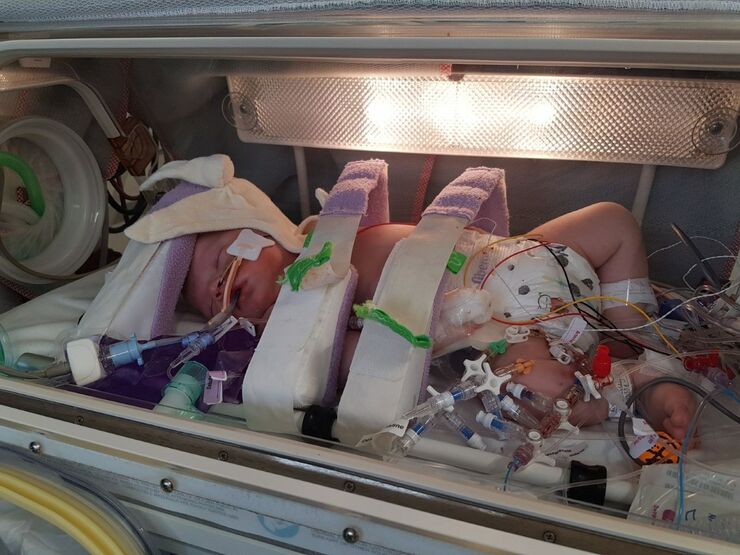
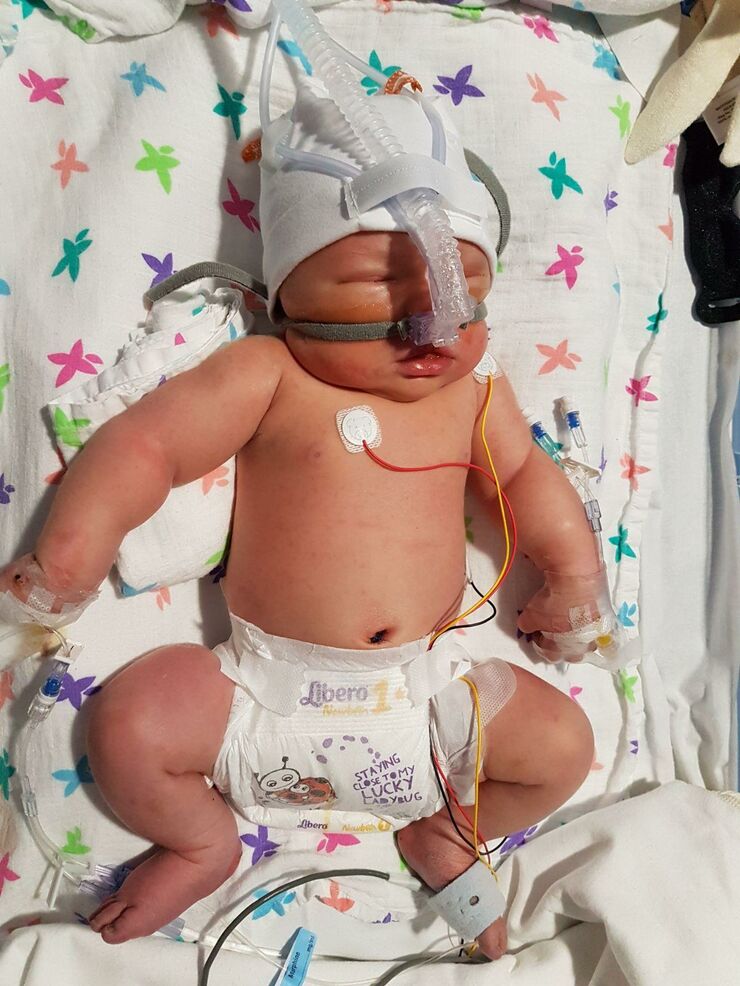
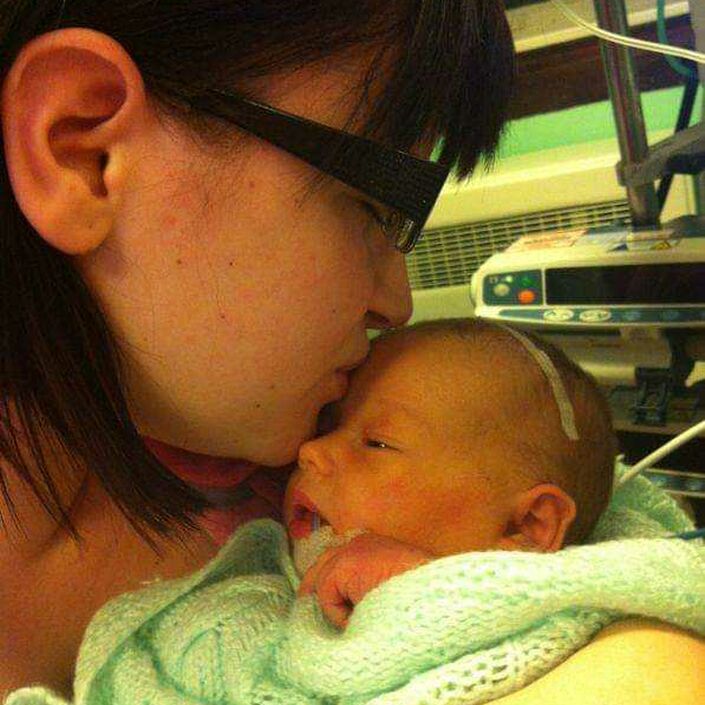
Considering the fragility of her condition upon admittance to NICU, Blake made a miraculous five-day recovery. She was soon discharged back to our local SCBU where we spent another five days establishing oral feeding.
Initially, Blake took to the bottle well and had her NG tube removed before we were discharged. However, a few weeks after we settled at home, she began displaying feeding difficulties which gradually got worse and by two months old, she would scream at feeding times and totally refuse the bottle.
We explored many avenues with the GP, however this very quickly turned into a severe bottle aversion. This pushed our ability to bond even further away, as feeding time is usually the main bonding time for parents and their babies.
I spent my time very anxiously and paranoid about how little Blake was drinking, and the trauma of it all combined with our birth/NICU experience led me to suffer from severe, crushing postnatal depression (PND), as well as post traumatic stress disorder (PTSD).
None of this was what I expected when becoming a mum aged 20, and the whole experience was very damaging to our bond.
We were thrown into a life we never imagined, full of appointments, diagnoses, medical professionals and terminology. We had so much to digest and come to terms with; the stress totally distracted me from being able to focus on bonding. In fact, it pains me to say that it took around 18 months to even start to feel a bond building.