Happy and healthy, I was 25 and preparing for the birth of my first baby. I attended all the antenatal support and breastfeeding classes eagerly awaiting the birth of my precious bundle on 7th November 2012.
On the evening of 11th November, I called the Royal Gwent Hospital, Newport as my waters went and they asked me to go in and be checked. They kept me in overnight with the plan to induce me, should labour not begin naturally.
I was induced on November 12th at 7am, which then led to the longest day of labour until 10pm, when things took a turn for the worse.
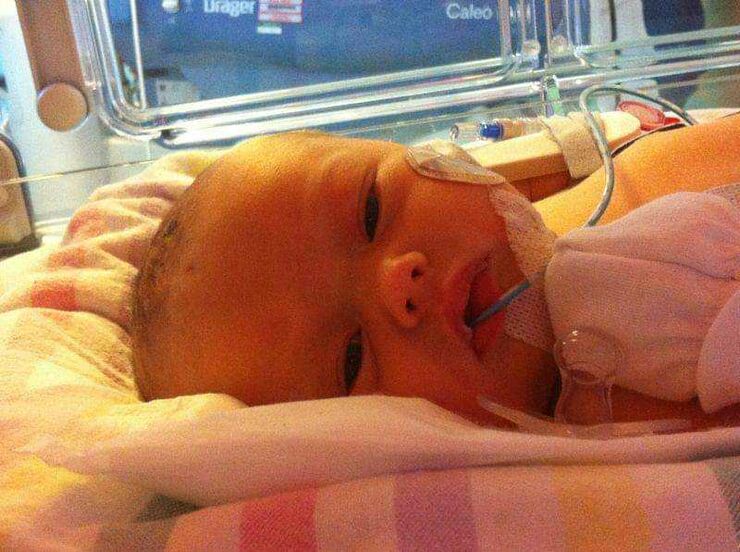
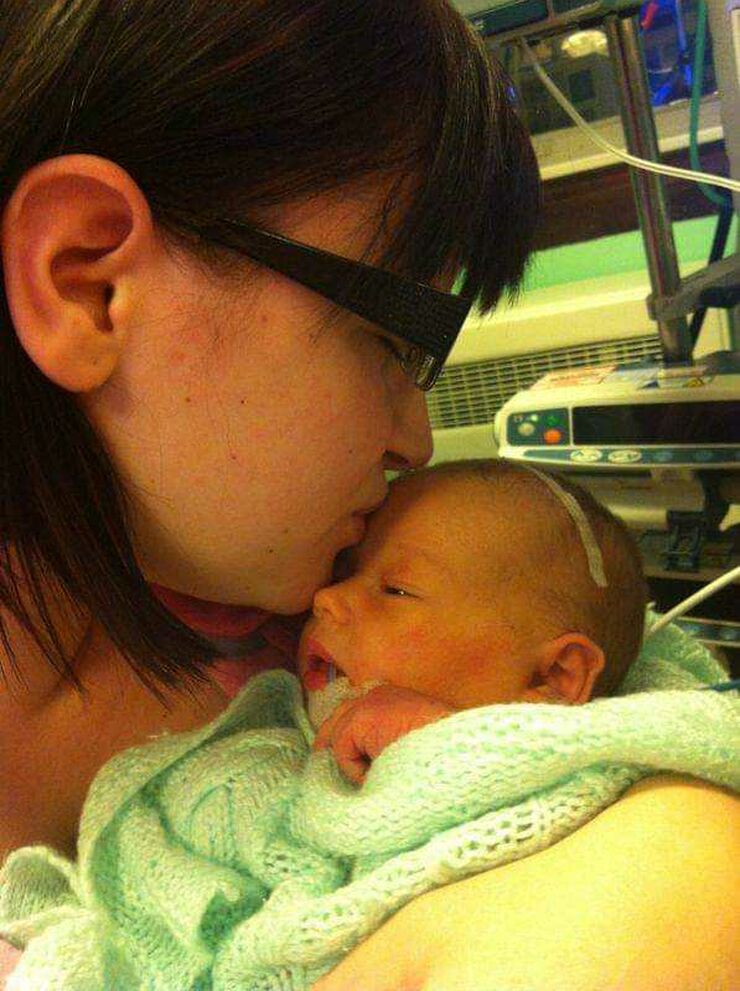
The room filled with doctors and nurses and I was taken into theatre as my baby had stopped breathing. I was given a spinal block and prepared that my baby was going to be taken straight to NICU for support.
What is NICU? I didn’t even know.