Before I started working on the Special Care Baby Unit at St Mary’s Hospital on the Isle of Wight, I was an adult coronary care nurse, who had no clue what went on inside a neonatal unit. That all changed when I fell pregnant with twins in 2016.
Because of pregnancy complications and likely prematurity, I was told throughout my pregnancy that my babies may end up needing to go to the neonatal unit. And when, after a scan at 26 weeks, I was put on bed rest due to the risk of premature labour, I was given a tour of the unit. The atmosphere was friendly and homely, but clean, busy and professional all at once. It was a whole different world, tucked in a little corner of the hospital that I, like many others, never even knew existed.
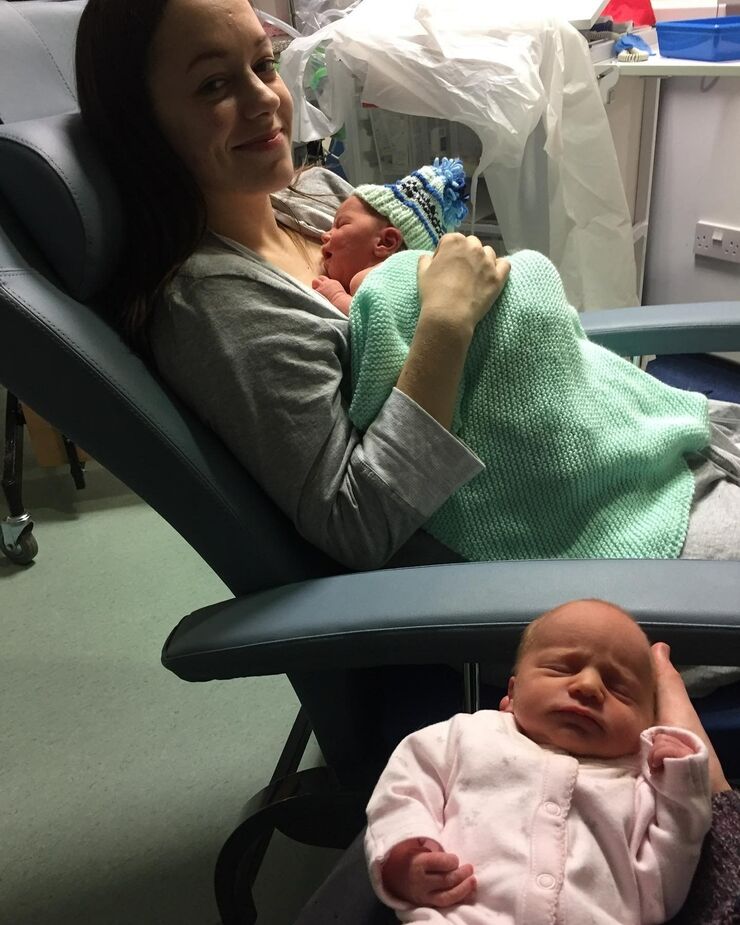
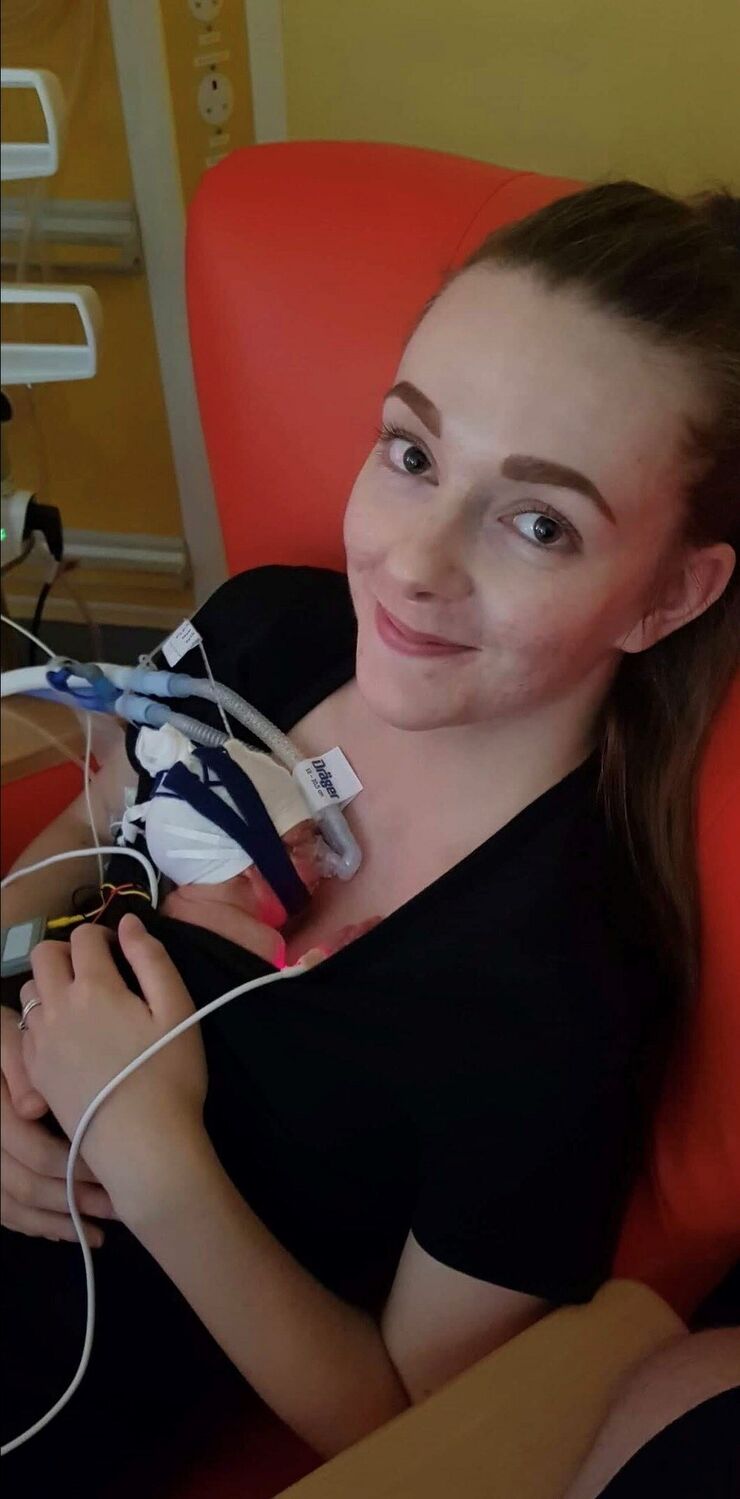
In January 2017, after ten weeks of bed rest, my twins were born by elective c-section at 36 weeks' gestation. My son was admitted to the neonatal unit with respiratory distress syndrome and sepsis. I was heartbroken, scared and exhausted, but the support we received from the nurses on the unit was exceptional.
He spent five days on the unit in a high dependency cot before being reunited with his twin sister. I often thought about what a wonderful job our nurses had done as I settled into life as a new mum of two tiny babies.