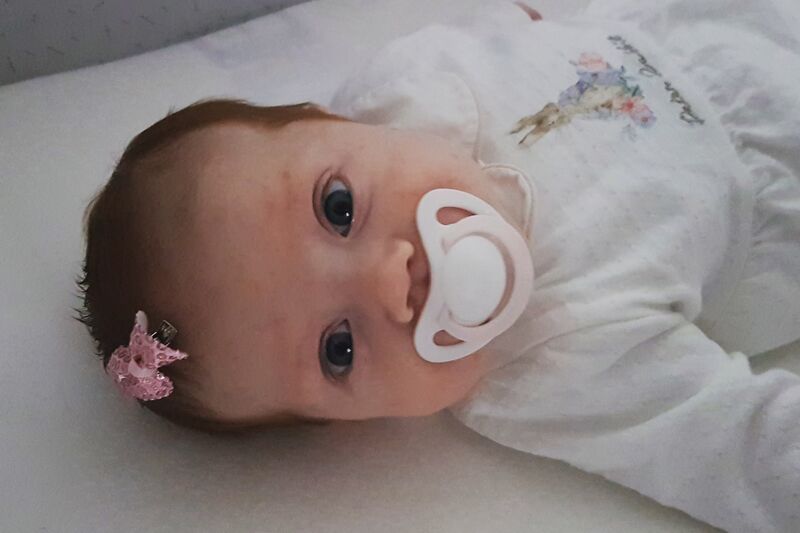
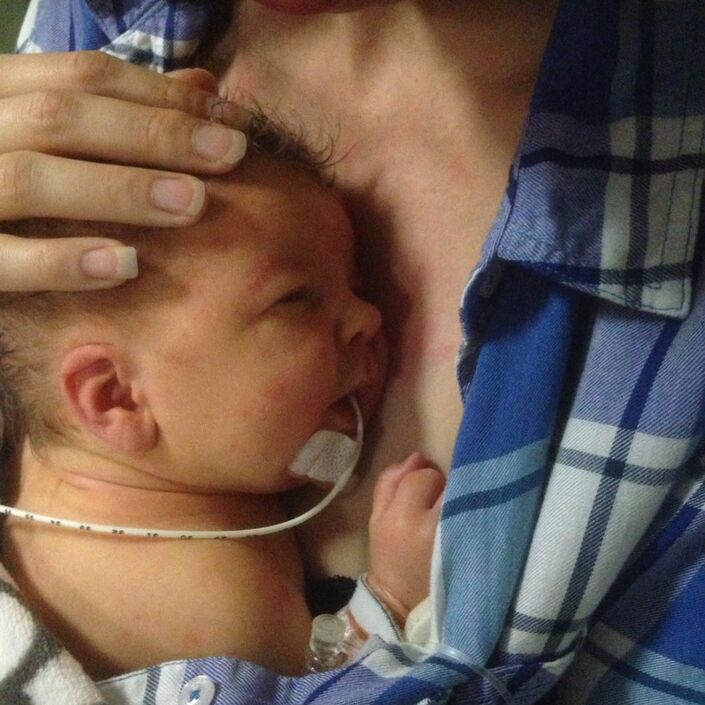
My daughter Poppy was born after a very long and traumatic labour. She spent a few moments on my chest before being whisked away as she had stopped breathing.
A team worked on Poppy for around 20 minutes before she was breathing again. I thought that once they got her back the nightmare would be over. Little did I know it was just beginning.
Poppy’s dad, Drew, was allowed to give her the first bottle. Every time he tried though, the milk would come back out of her nose and mouth. It happened again when the midwife had a try, so she said she would take Poppy to get looked at to see if she had any mucus blocking her airways. In the meantime, I was taken into theatre to have my placenta removed.
After my surgery, I was told that Poppy still wasn’t feeding. The staff were trying different types of formula to see if any of them would work but to no avail. The midwife then noticed that Poppy didn’t seem to be able to hold her saliva in her mouth so said she would take her back to NICU for the doctors to take another look.
Hours dragged by. The midwife finally returned to tell me that Poppy would be transferred to the Royal London Hospital within the next hour.
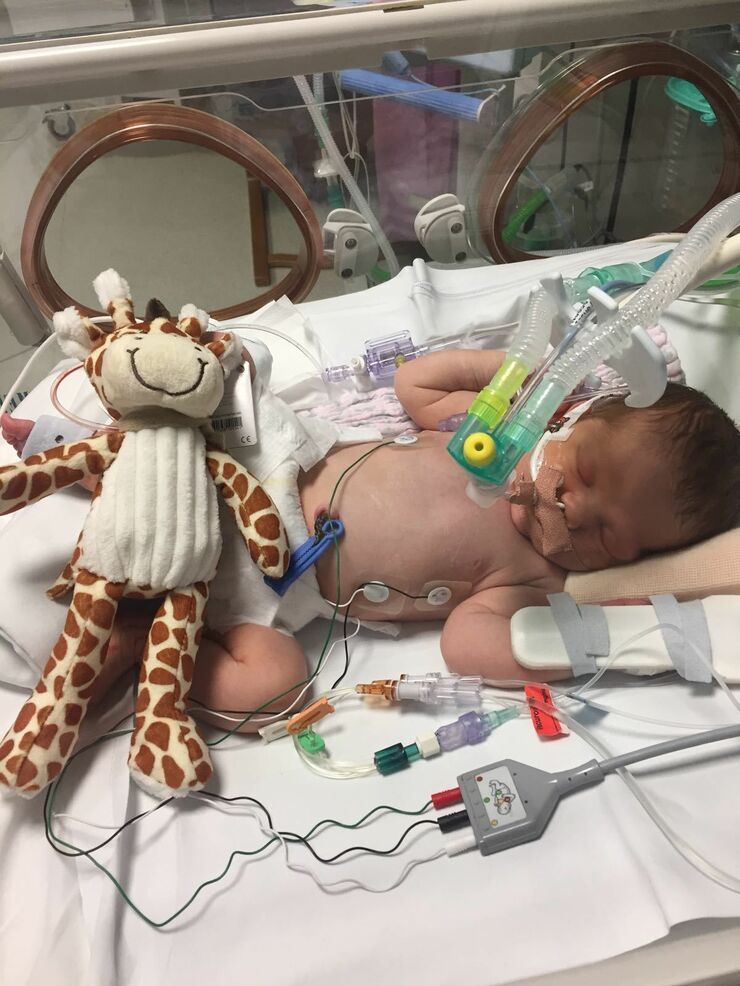
Drew and I went down together to the NICU to find out what was going on with our daughter. The doctor told us that they had been unable to fit Poppy with an NG tube so had done an x-ray to figure out what the problem was. The x-ray revealed that she had Oesophageal atresia (OA) and tracheo-oesophageal fistula (TOF).
OA is a rare birth defect that affects a baby's oesophagus. The upper part of the oesophagus doesn't connect with the lower oesophagus and stomach. It usually ends in a pouch, which means food can't reach the stomach.
TOF causes air to pass from the windpipe to the oesophagus and stomach, and stomach acid to pass into the lungs.
These defects mean the baby – our Poppy - won't be able to swallow safely, if at all.
These medical terms are so familiar to our family now but when we were told about them that day, we couldn’t remember what was said. My head was fuzzy from all the drugs from my operation and I was too tired to take any of it in. I was taken back to the ward whilst Drew stayed with Poppy until the transfer team arrived. He watched our baby be blue lighted off to another hospital, unsure of whether or not she’d make it.