I had never given too much thought to breastfeeding. I’d read it was exhausting but I assumed that I would do it because I thought that all my baby would need to do was latch, drink and repeat. But since when was anything to do with a baby so simple?!
My son was diagnosed with severe intrauterine growth restriction (IUGR) at 30 weeks. After five weeks of what felt like constant visits to the maternity unit for monitoring, we were told that our very little man would be joining us immediately. It was difficult to be told that our baby was better out than in – it felt like it was just too soon.
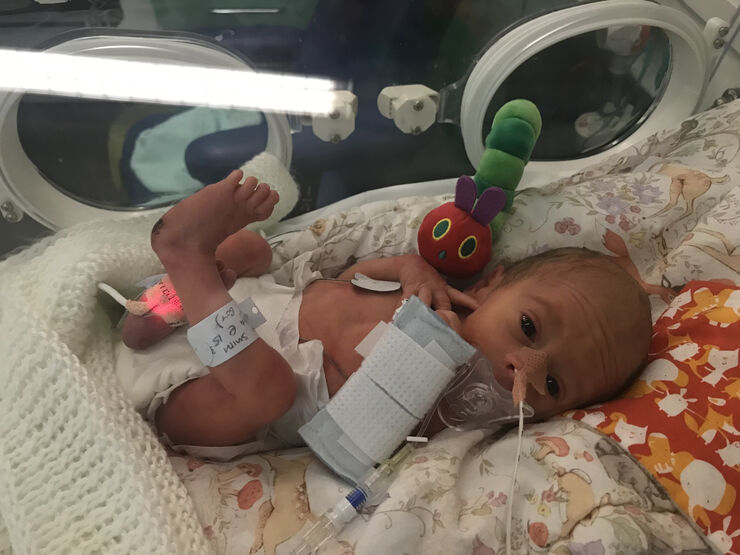
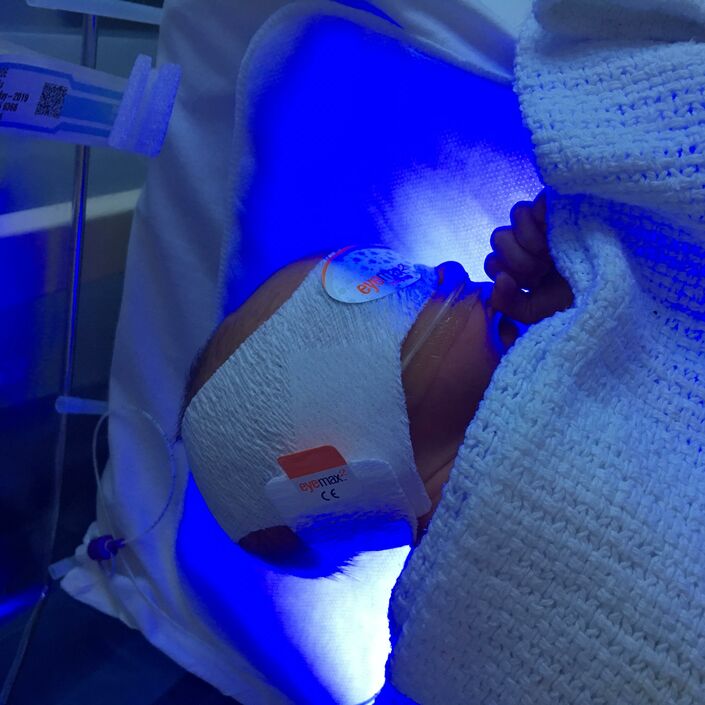
The birth and the hours – days even – afterwards felt like a complete out of body experience. James was born at just over 3lbs, and after a quick peek he was whisked off to the NICU while I was wheeled into recovery with my bewildered husband following closely behind. I was handed a couple of syringes with an instruction pamphlet on how to express for colostrum and we were left to it.
I didn’t know what to expect from this first session of expressing, but I certainly imagined I’d be able to produce more than a few drops. I always feel a bit sad when I think of my husband helping me scoop up that tiny amount with the syringe.