Watching your baby
It is really important to spend time getting to know your baby. Sometimes you might feel like you spend a lot of time just looking at them.
Watching your baby can help you to learn how they show signs they might be uncomfortable or in pain, as well as being calm and content. This can help you to know what you can do to soothe and comfort them.
Combined with your natural intuition as a parent, watching your baby will help you to help the doctors and nurses. Together you can tell when your baby might not be feeling very well, or might be in pain. The unit should have a place for you to write some of this information in your baby’s notes.
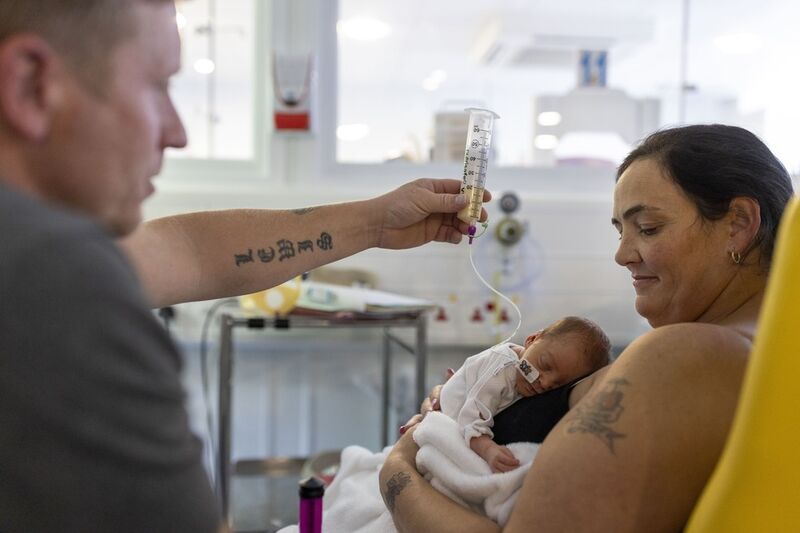
Skin-to-skin
Sometimes called ‘kangaroo care’, skin-to-skin means placing your baby undressed onto your bare skin on your chest, so that your skin touches. This is shown to help you to connect with your baby, as well as calming your baby if they are feeling pain or stress.
It also has been proven to help your baby’s sleep, growth and has other physical benefits. Mums, dads, brothers, sisters and other family members can do skin-to-skin.
Staff will let you know if your baby is ready to have skin-to-skin with you – sometimes you might need to wait until they are more stable.
The team will help you to get your baby onto your chest. This might take a little time if your baby is attached to wires or a ventilator. They will show you how to support your baby and make the most of this time together.
For kangaroo care to really benefit your baby, it’s helpful if you can do this for at least one hour if possible. Make sure you are really comfortable, and have everything you need before you start.
For more information about skin-to-skin care, visit our page - Skin to skin and kangaroo care.