Mila was our second baby – her birth was fairly quick and very straightforward. In fact, it was exactly how I had wished.
I was having mild contractions whilst putting our three-year-old to bed and went to hospital around 11pm, giving birth at 2:20am in the pool with no interventions.
Everything went so well that we were preparing to go home by lunchtime. I sent my husband home around 5am so that he could get a couple of hours of sleep and our son would wake up with him there. I tried to rest knowing the first night at home is always tough for feeding.
As I did with my son, I was planning to breastfeed, so Mila was latching on every hour or so. I noticed that her breathing had started to be quite noisy and she was grunting, but she didn’t seem breathless particularly – I mentioned to the midwife who agreed but also didn’t seem concerned.
Mila was due to have her newborn examination test before going home. Ours was completed by a lovely midwife, who agreed that her breathing was noisy but thought it was possibly a blocked nose, as her chest was clear and her oxygen levels were good.
I had a gut feeling that something wasn’t right, and I still wasn’t reassured and asked for a paediatrician to review before we went home. The first paediatrician agreed and admitted us to the ward overnight so she could be monitored. She was going to ask her senior to review Mila too.
There was no panic or rushing around - everything seemed quite calm. I thought Mila was maybe a little mucousy and hoped this would clear in a couple of days.
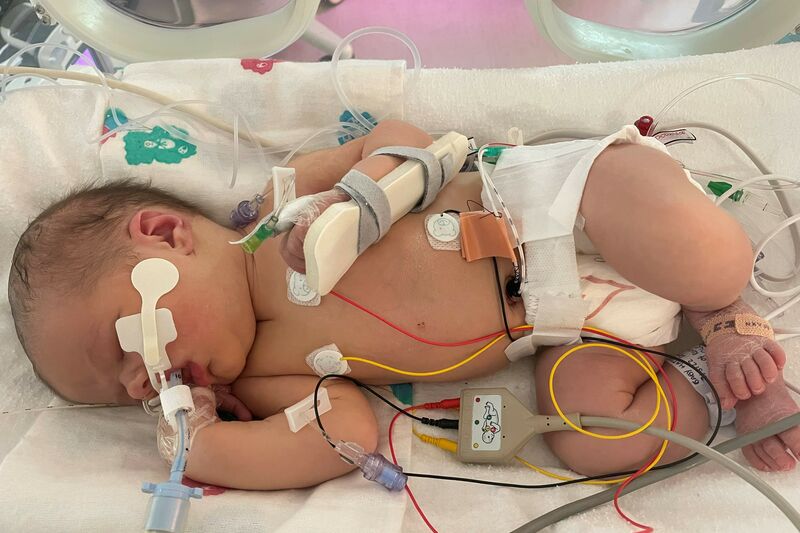
I told my husband who was just about to leave home to come back in. The senior paediatrician arrived to review her and within 30 seconds of examining her, made the decision to take her around to NICU.
I can’t remember the conversation exactly as it all happened very fast, but she said that she thought my baby was struggling to breathe more than we first thought. She added that I should give her a quick kiss and a cuddle, but they were going to take her to NICU and would come back to me once she was in her incubator.
It’s all a bit of a blur now, but I remember my heart sinking, feeling nauseous and a million thoughts racing. I dressed Mila back in her baby grow as tears fell, which now seems silly as I knew they were going to take her baby grow straight off again, but I was on autopilot.
The midwife left to update the team, I imagine and get the notes, so I was left alone. They had taken my baby.