In 2018, I experienced complications during my first and only pregnancy at 17 weeks and was informed following my 20-week scan that I had cervical ectropian (cervical erosion), which is when cells from inside the cervix grow onto the outside of the cervix. I was told that this can be common during pregnancy and shouldn't cause any other issues.
Then at 21 weeks and 3 days, whilst at work, my waters suddenly went. After looking online at my symptoms and assuming it was definitely the former, I contacted the hospital and drove myself there. It was confirmed in the maternity assessment unit that I had experienced Preterm premature rupture of the membranes (PPROM). I was told it was extremely likely that I would go into labour within 48 hours. I was treated for suspected sepsis and given IV fluids and antibiotics, to help avoid infection and moved to the labour ward for regular monitoring.
My husband was working hours away, but my parents came to support me. My twin sister is a community support worker in the maternity ward and had seen my name on the board. She rushed in to see me. When I saw that she was worried, I found it really upsetting, but I also felt extremely lucky to have my family there to support me. I can remember speaking with a consultant and asking him if I would have a miscarriage. He said that he couldn't answer that question but explained that I was very likely to go into labour, and if this happened, given how early in my pregnancy I was, it would be very difficult for my baby to survive. I explained that I just wanted my baby to be ok.

After 48 hours on the labour ward, nothing changed, other than the continuing leaking of my amniotic fluid. My cervix remained closed and my baby’s heartbeat remained strong. It was confirmed that our baby didn't have much fluid around them. The doctors had said they had seen other pregnancies continue to a further gestation following PPROM, but they also explained that I was now at an extremely high risk of infection, so it was a very uncertain situation.
A consultant spoke to us regarding our options going forward and informed us of the risks with continuing with the pregnancy, such as a risk of serious infection to both myself and the baby, the risk of our baby being born with pulmonary hypoplasia (incomplete development of the lungs), limb contractures, cerebral palsy, and many other risks associated with a premature birth. We were told that it was very likely that our baby could be severely disabled. But we were also told that it was possible to continue with the pregnancy and for me to be closely monitored to see what happens.
After a brief discussion, my husband and I decided that we wished for our very much wanted baby, to be given every chance at life. We therefore decided to continue with the pregnancy and do everything we could to protect our baby and reach as far along as possible. I did some online research whilst in hospital, after being recommended a charity through a friend. The name of the charity is Little Heartbeats and they proved to be the most amazing support and lifeline during the most difficult time in my life. The lady, Ciara, who runs the charity is incredible and gave me so much support and guidance. Little Heartbeats also sent me an information pack, which included a bear to record my baby’s heartbeat. This meant more than anything, as I knew that whatever happened, I would always have a recording of my baby’s heartbeat.
I was allowed to go home after 48 hours and given a 10-day course of oral antibiotics. I was also told to take my temperature every 4 hours and to look out for signs of infection. I was advised to get signed off work and told to avoid anything that could pull on my tummy, such as hoovering and walking my dog. I was monitored with weekly blood tests at the hospital and given a growth scan for the baby every 2 weeks, as well as the fluid levels around the baby being monitored. The plan was to get as near to 34 weeks gestation, when the doctors would look to induce me, as they didn't want me to go any further.

During the next 9.5 weeks, I was admitted a few times for bleeding and reduced movement and was given steroid shots at 27 weeks to help with the baby’s lung development, in the event that I needed to deliver.
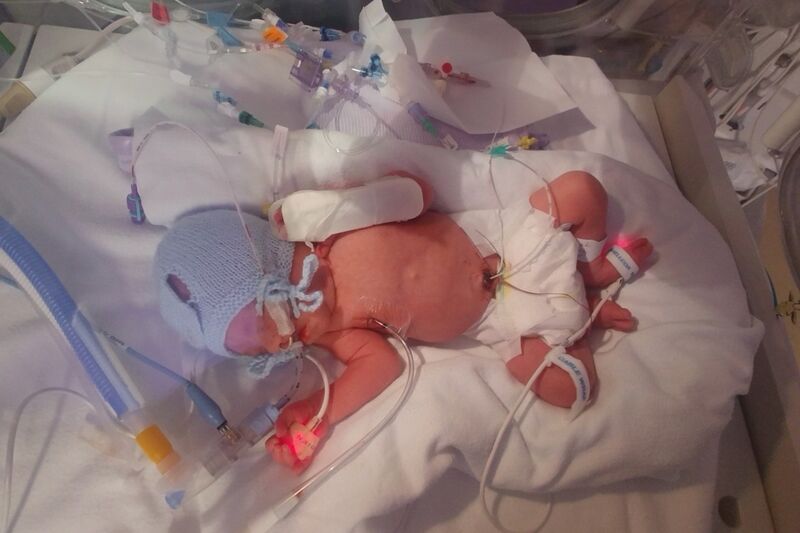
We ended up making it to 31 weeks exactly, following my last hospital admittance for bleeding. I was given magnesium sulphate, a drug administered to help reduce the risk of cerebral palsy and bleeds on the brain for the baby. I then delivered my son via C-section due to placenta abruption. Although extremely anxious, my birth was very calm and such a wonderful experience. Our son, Jax, was born at Queen Alexandra Hospital in Portsmouth, weighing 4lb 3. He let out a little cry when he was lifted out, which was very reassuring, but was resuscitated a couple of times very soon afterwards and intubated in theatre. He was then wheeled past us where we got to see him for a few seconds before he was taken to the NICU.
We named Jax after the midwife who looked after me following the PPROM diagnosis. We realised the name Jax meant 'God has been gracious, has shown favour', which felt even more fitting at the time.
After my C-section, we waited on the maternity ward for an update, for what felt like forever. We were told by a NICU doctor that our baby was extremely poorly and critical. He said that he was not able to tell us at this stage if Jax would make it through. We were unable to see him, so just had to wait. Hours and hours passed. When I finally got a visit from the same NICU doctor, he informed me that Jax was still extremely poorly but said the team had managed to stabilise him and offered to wheel me around to see him.
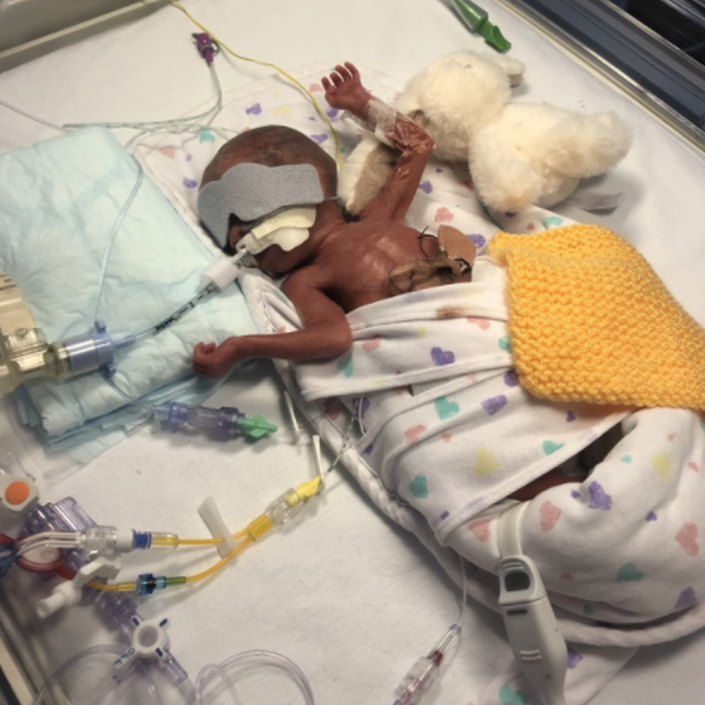
As this was now the early hours of the morning, I decided to wait until my husband arrived at 9am, so we could meet our son together. I wish now that I had been brave enough to see him on my own. The NICU doctor offered to take my phone to Jax, so he could take some photos for me. I can't explain how grateful in that moment I felt. He came back with some photos and explained what all the tubes and wires were and answered any questions I had.
Seeing my son in an incubator, intubated with tubes and wires everywhere was heartbreaking. His little body was shaking and vibrating from the oscillator ventilation, and I couldn't believe how many different medications were being pumped into his tiny body to keep him alive.

Jax spent 60 days in NICU and overcame pulmonary hypertension, Patent ductus arteriosus (PDA), battled a couple of different infections, received 3 blood transfusions, had talipes in both feet (one was a lot more severe), had positional plagiocephaly and chronic lung disease. He came home on oxygen and required this until he was 10 months old but is the most amazing happy and smiley little boy, who is now nearly 3 years old.
Jax is still under the care of a consultant in Southampton for monitoring of his talipes but no operations have been needed, just physiotherapy. He is currently on regular steroid inhalers to help his lungs and has some very mild developmental delay surrounding his speech, but Jax has defied the odds against him.
My experience greatly affected my mental health and I ended up with PTSD and anxiety, but I would go through all of it again and more, knowing the end result would be having our amazing son in our lives.
We owe everything to the amazing maternity staff, NICU nurses, doctors and consultants at QA Portsmouth, who looked after us all throughout our journey. We are forever in their debt.