Nothing about my pregnancy was straightforward. IVF, pre-eclampsia and HELPP syndrome all meant that I didn’t get the chance to enjoy any of it.
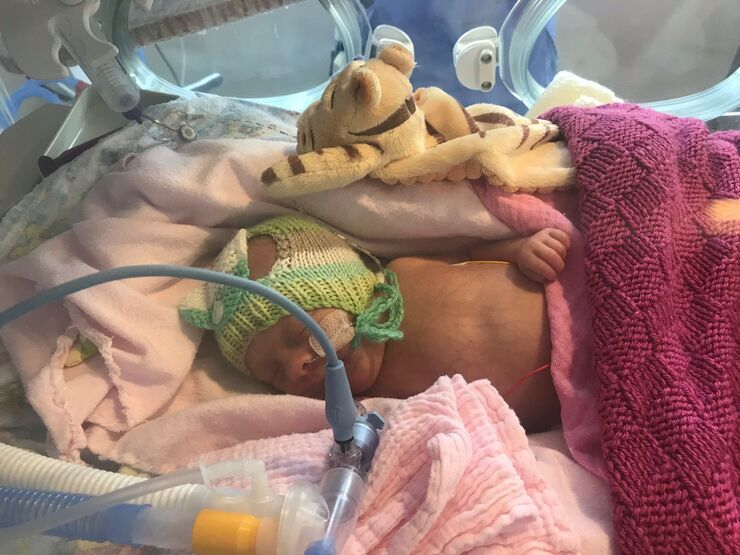
In order to save both our lives, my daughter was delivered via emergency c-section at 29+2 weeks. Frances did brilliantly well at first. She spent three and a half weeks at a NICU in Portsmouth before being transferred to our local hospital in Chichester. We were doing really well. I was aware of how fortunate we were that our daughter was such a strong little fighter.
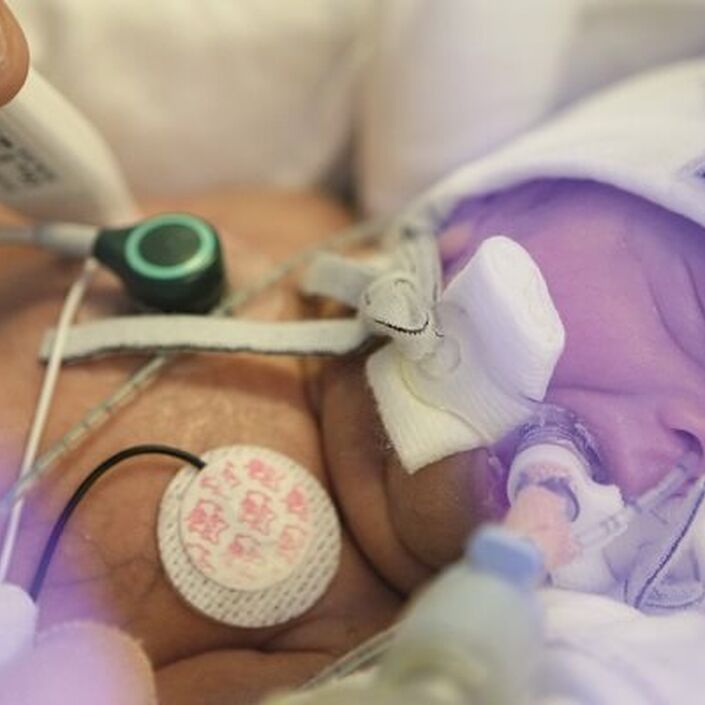
Then that rollercoaster ride took a massive drop. Following her routine ROP test. Frances stopped breathing. She’d had a rare reaction to the eye drops, which led to her being intubated and moved into the intensive care nursery. The doctors and nurses were amazing. They reacted so quickly to stabilise her and make her comfortable – Suzi her primary nurse didn’t leave her side all day.
While this was all happening, I was at another part of the hospital having a check-up appointment and my husband was at work; our baby girl was on her own. I received a phone call from the unit, the minute the number came up on my phone I knew something was wrong and I didn’t take a breath throughout the call. I was scared, anxious and just wanted to get back to Frances. No matter how much they reassured me she was fine I had to see her for myself. Running across the hospital, I rang my husband feeling panicked and upset. I told him to get to the hospital as soon as he could. The worst thoughts were running through my mind. I was terrified of losing her and felt utterly helpless, knowing there was nothing I could do to change the situation.