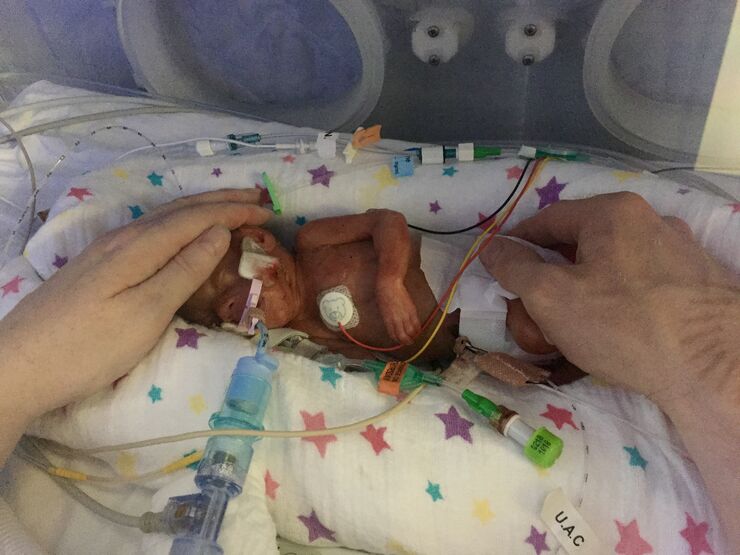
Alongside using the fantastic nurses and practitioners as a means for support, we very quickly aimed to cope better.
Some of the strategies we found useful were:
1. Developing a flexible routine
Each evening we’d plan the next day, ensuring we included time for breaks from the NICU. We accepted that we may not do what we want to do at the specific times – but by writing the plan down, each task or activity most often got done at some point during the day.
2. Making time to talk
We talked over a coffee each morning, allowing each other time to vent. We made a rule: “No interrupting each other and no judging what the other person says”. This helped us get everything off our chest without penalty.
3. Accepting help
We were at first reluctant to accept help from our immediate family, but their support through doing our laundry, cleaning and sometimes preparing food was invaluable – it allowed us to focus on supporting Nancy.
4. Talking in future tense
We insisted that the practitioners discussed what the plans were for Nancy the next day or week, which constantly reassured us.
5. Managing visitors
Our family were vising many times a day because we had told them that the NICU had an “open visiting schedule”. Escorting them up to the ward regularly became stressful as we didn’t have as much time for ourselves. We then dictated the schedule that worked for us.