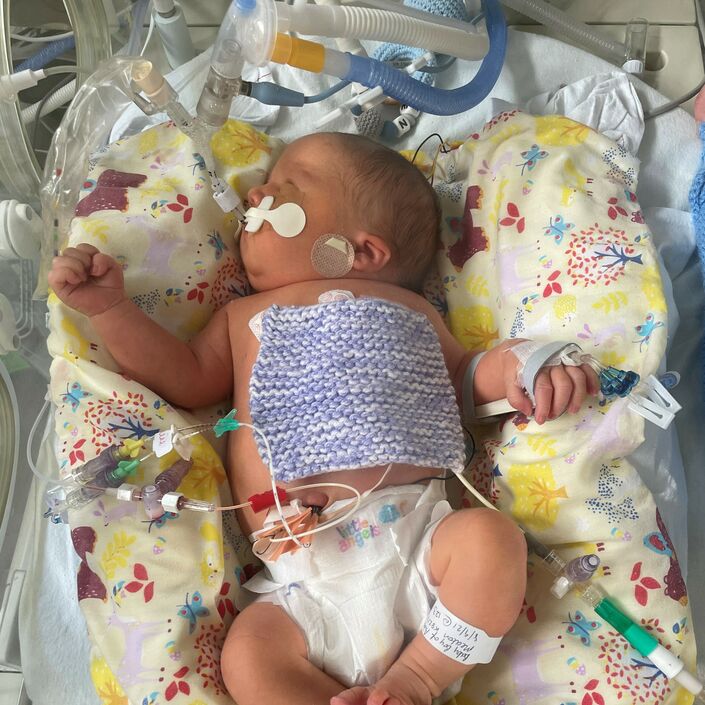
I had gone into the hospital at 38 weeks and three days with reduced movements, this being my fourth episode in about six weeks. It was a Friday morning and I was hooked up to all the monitors, which showed that our little girl was moving and had a strong heartbeat.
However, because it was my fourth episode of reduced movement, they wanted to induce me then. A few days had passed and I was struggling to dilate, even after many pessaries and a hormonal drip. At this point, I was getting really disheartened and wondered what was wrong with me.
At 11 pm on Monday, they decided to perform an emergency c-section. They opened me up and became clear to them within five minutes that my baby was impacted in my pelvis, which was a neonatal emergency.
While trying to get her out, my placenta started to come away in chunks and abrupt. An inverted T incision was performed along with a doctor pushing up through my vagina to get her out and she was pulled out breech. Our daughter was finally born at 00:55 am, an hour and a half later.