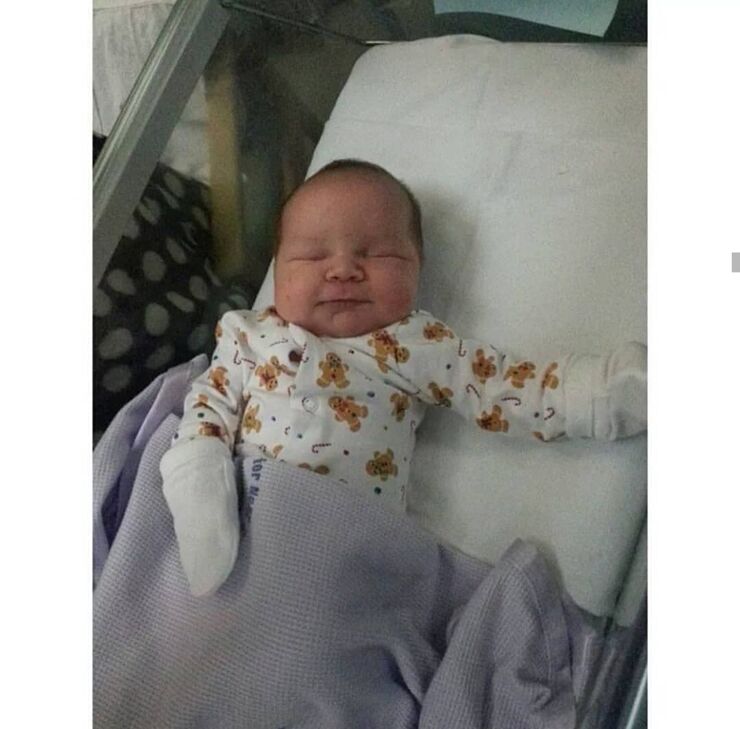
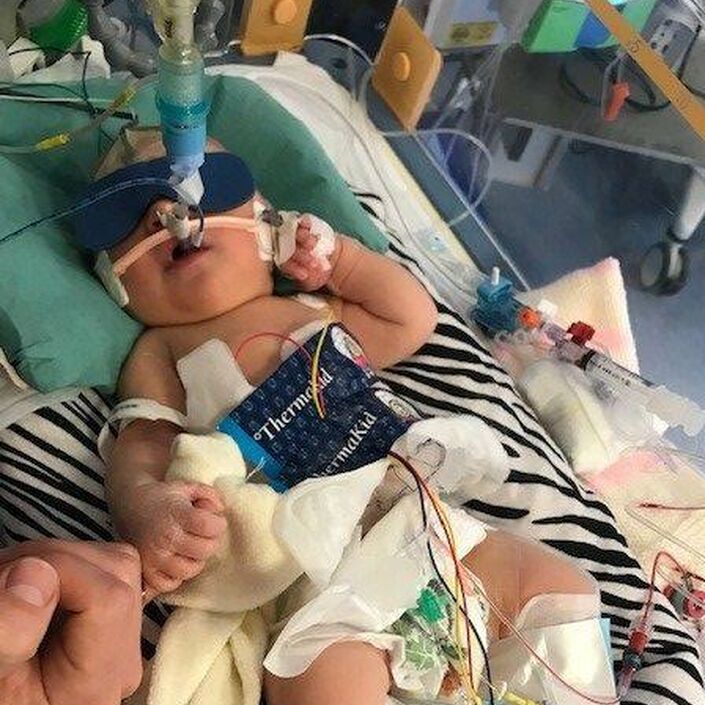
After this information overload, I remember bursting in to tears and asking to be taken out of the unit. I felt like I'd failed my baby so completely, and I couldn't bear to look through the plastic separating us. This wasn't how it was supposed to be! Full term babies don't end up on neonatal units! But they do, and mine did.
As I was so poorly, I was lucky in a way that I stayed at hospital for the same amount of time as Ted. That's not to say it didn't have its difficulties. Having had a c-section, my mobility was restricted to begin with and fitting in all my own medication for sepsis and blood loss took up a lot of time. I had one fantastic midwife who would bring my pain medication to the NICU so I didn't have to miss out on precious moments with Ted.
I won't ever get the dark hallway lights or the lonely lift rides at all hours of the night out of my head. It was Christmas time, and I remember the nurses decorating the unit, a bittersweet reminder of what we were missing on the outside world. I'd often ask if we'd be home for Christmas, but doctors had already decided Ted needed 3 weeks of antibiotics, so it was completely off the table. Whilst pregnant I dreamed of my baby's first Christmas, I was due on the 15th so assumed I'd be home well before. It felt like yet another parental milestone to grieve for.
In total Ted spent 2 weeks in the neonatal unit. He was given 4 different types of antibiotics, had an ng tube and a longline that went from his ankle to his heart. It is the most disorientating thing to be sat next to a plastic box containing your baby, surrounded by machines with their different numbers and beeps. I used to watch his antibiotic timer go down, desperate for the next cuddle. I will never not feel guilty for not being able to be there for some procedures he needed, but I found things like blood tests incredibly traumatising to watch. He was my baby, and there was nothing I could do to help or make it stop, whilst knowing it was extremely important.
On the 23rd of December, Ted's long line stopped flushing. The doctor's debated and decided he had improved so drastically that we could go home. In itself this was a challenge for me, as I wasn't sure how I'd be able to look after him without the reassurance of machines and nurses surrounding us. It really was a surreal moment to be able to take him out of the unit for the last time.
I am really pleased to say that Ted has no long lasting effects and is a healthy 4 year old little boy, who loves playing football, horse riding and playing with his little brother. We are incredibly lucky.
I still struggle with remembering our neonatal journey, it isn't what you expect when you have your first baby. Although I recognise that I am beyond lucky to have a healthy happy child, the mental health aspect still affects me nearly 5 years on. My advice to neonatal parents, past and present, is to be gentle with yourself. It is so easy to blame yourself, or tangle yourself up in what ifs. Neonatal parenthood isn't what anyone would choose, but I'm glad there are charities like Bliss who are there if support is needed.