I’ve wanted to be a Mum for as long as I can remember, so at the age of 38 - still single, and clutching fertility test results that told me my time was running out, I decided to go it alone and attempt to become a solo Mum by choice (SMBC). After four difficult rounds of IVF using donor sperm, I fell pregnant.
My pregnancy went really smoothly and as I sailed past 37 weeks I naively thought I was home and dry. How wrong I was. In November 2022, at 39 weeks, my consultant recommended induction and after three tough days on the induction ward at Worcester Royal Hospital, my pregnancy ended in a frantic emergency c-section.
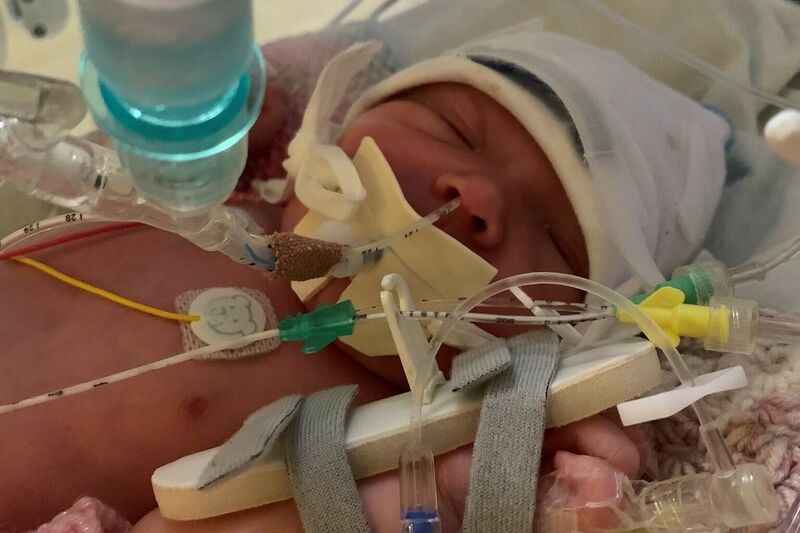
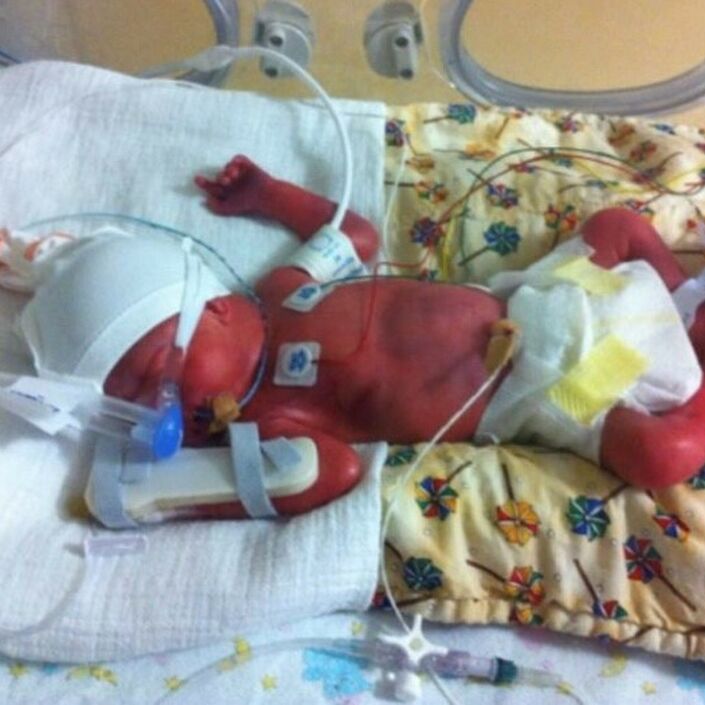
My daughter Alice was born in very poor condition and required 25 minutes of resuscitation - the longest and most traumatic 25 minutes of my entire life. I was quickly told that Alice urgently required cooling therapy to try and minimise damage to her brain, but that it wasn’t available at Worcester and she needed to be transferred to a level three neonatal unit.
The nearest available bed was in Wolverhampton New Cross Hospital - 42 miles and one hour away. It was made very clear to me, and my family, that Alice was in a very critical condition and may not survive. Alice was transferred that evening, and I followed in an ambulance a couple of hours later - distressed, disorientated and under sedation. I arrived to find Alice settled in the NICU, wired up to numerous machines and monitors.
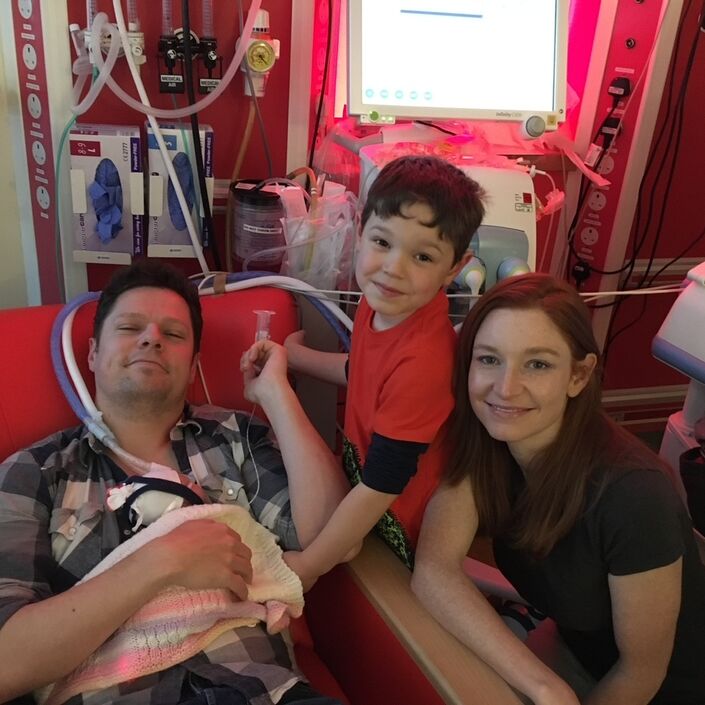
As I had undergone a c-section I was also admitted to New Cross. However, with my physical recovery going well, I was discharged on day three. Alice was so poorly and I was still in shock and very traumatised - and a long way from home - so I was told a bed would be made available for me in a ‘flat’ on the NICU ward. This made a world of difference to both me and my mum, who had been my birthing partner and had stayed by my side throughout. Mum was treated in exactly the same way as a traditional ‘dad’ would have been, and that acceptance of my circumstances and support for her was hugely appreciated by us both.
The flat was just a small room in the NICU ward, but every effort had been made to make it comfortable and welcoming for families going through the worst time of their lives. Being in the flat meant I could spend as much time as I possibly could with Alice - doing all of her care, feeding, talking to her, stroking her and just finding every small way possible to bond and be her mum.
It also meant I could be present for every ward round. I could listen and ask any questions I had so I didn’t feel I was missing anything. Occasionally I left the hospital to grab a coffee in the retail park opposite and I found this so difficult - leaving the hospital without my baby felt unnatural – and the thought of having to go home for the night without her was unbearable. Being around so much meant I got to know the nurses well, but I didn’t want the nurses to look after her, I wanted to do it myself. She was my longed-for baby and I didn’t want to miss anything.