I was 23 weeks pregnant and had come into Guernsey's maternity ward for a check-up the day before as I felt something was not right. I'd been sent home reassured then but, on the Saturday, spent the day in considerable pain and went back up to the hospital that evening. After a scan, I was told that due to the risk of early delivery, I would be medevacked to Southampton where they hoped they would be able to stabilise the pregnancy and get my baby closer to term.
Perhaps I was naïve, optimistic or the medical staff did a good job about keeping it all feeling routine, but I really thought it would be a case of waiting out the boredom on bedrest until I hit 30 weeks and be transferred back to Guernsey to wait out as much of the pregnancy as possible. With me on a stretcher and an incubator onboard in case we delivered mid-flight, there wasn’t room for Gareth alongside the medical team so he followed later that day.
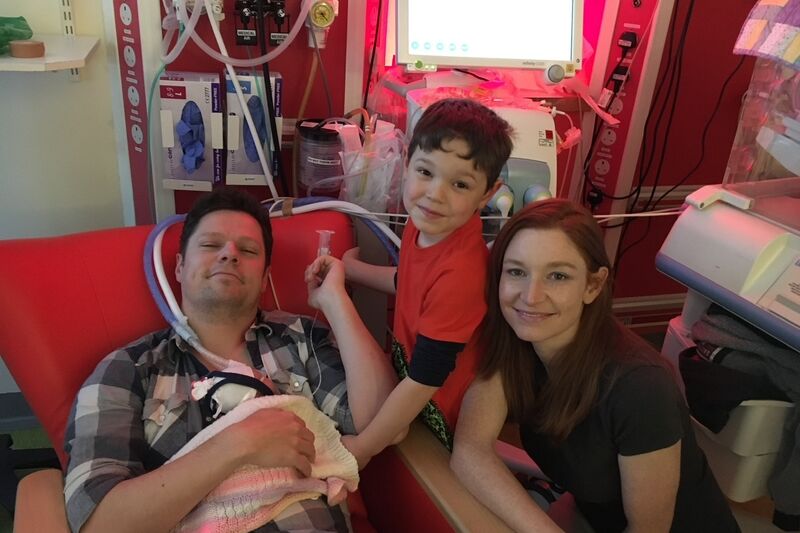
With what we thought would be a long bedrest in Southampton, my main concern was initially how I would be able to continue to make life as normal as possible for our then five-year-old son, Jasper, who would need to spend most of that period in Guernsey with his father so that he could continue to go to school, and worrying about how we would afford the plane tickets for him to come and visit me at the weekends.
The initial chaos of the transfer to Southampton had died down and Gareth flew back to Guernsey to be with Jasper. I got a subscription to an online postcard service so I could take pictures and get them sent as postcards so he had something arriving every day from me.
However, the long wait wasn’t to be and after just two more days in hospital, my waters broke and it became clear that despite my best efforts, the baby was coming.
The hours before delivery were extremely tough. The conversations with doctors and counsellors were all around survivability, developmental outcomes and the realisation that if Zara survived her birth - the ordeal she (and we) was about to go through - then Southampton was going to become our second home for some time.
We’d later find out the reason for my PPROM was that I had an infection of my uterus. This wasn’t discovered until the c-section, but I had suddenly developed a real, profound seizing fear which was a sign my infection was now sepsis.
I am so grateful that I and the medical staff listened to my instincts that something was terribly wrong. They moved fast and as we went into the operating theatre, the panic I had felt from the septicaemia ebbed away and I felt much calmer, I was in good hands. The anaesthetist explained they wanted me to take 10 deep breaths before I was put to sleep. They wanted the baby to get as much oxygen as possible before the anaesthetic reached them and the team would work quickly. I remember taking the biggest lung-bursting deep breaths of my life, conscious that it was the last thing I was going to be able to do for my baby before they had to take over the fight, all on their own.
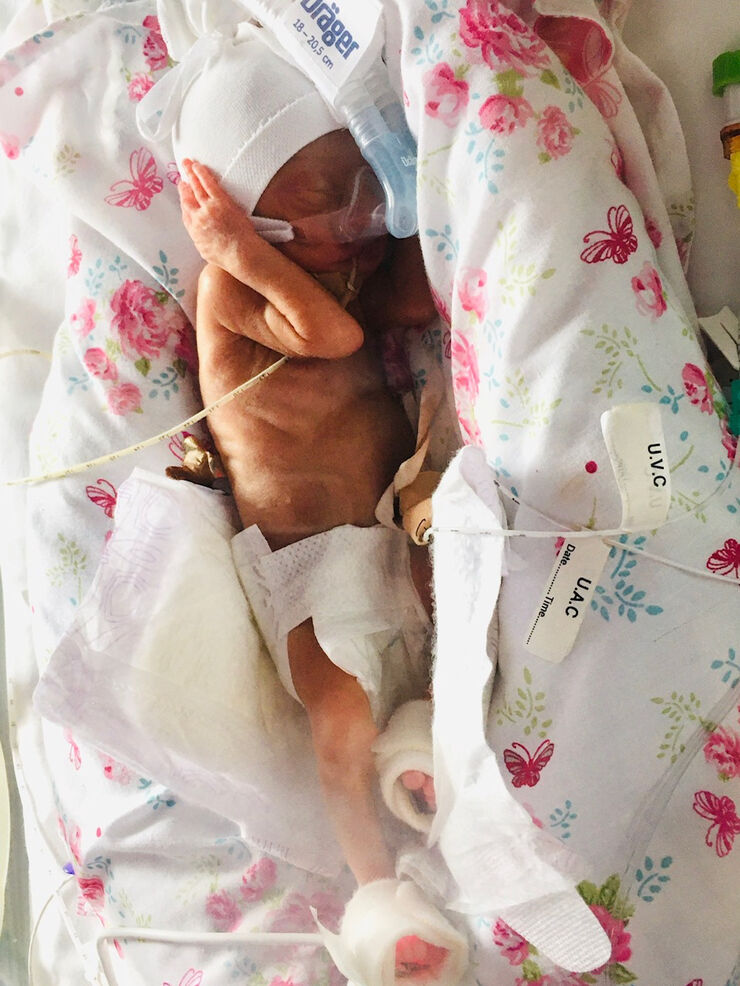
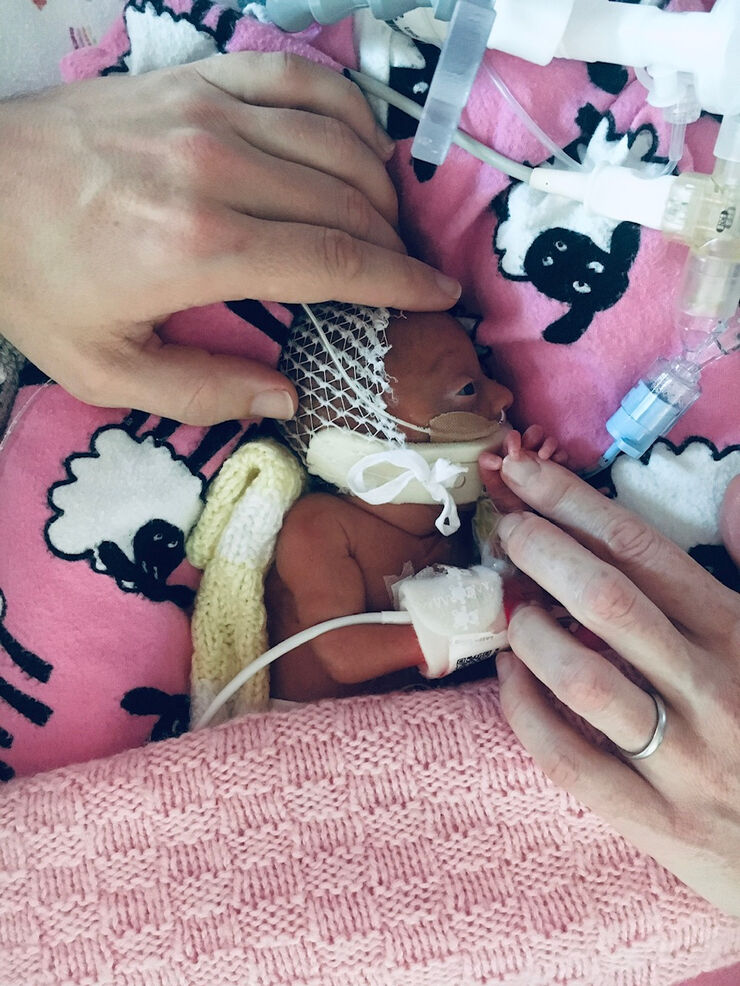
Zara was born by general anaesthetic c-section at 24 weeks and three days; around four months premature. Including medical equipment, she weighed 590g and measured 30cm long. She was resuscitated in theatre and placed in a plastic sandwich bag to protect her near-translucent skin from the outside world. As she was wheeled in an incubator to the NICU, Gareth got to meet her in a corridor, found out we had a little girl and he named her there.
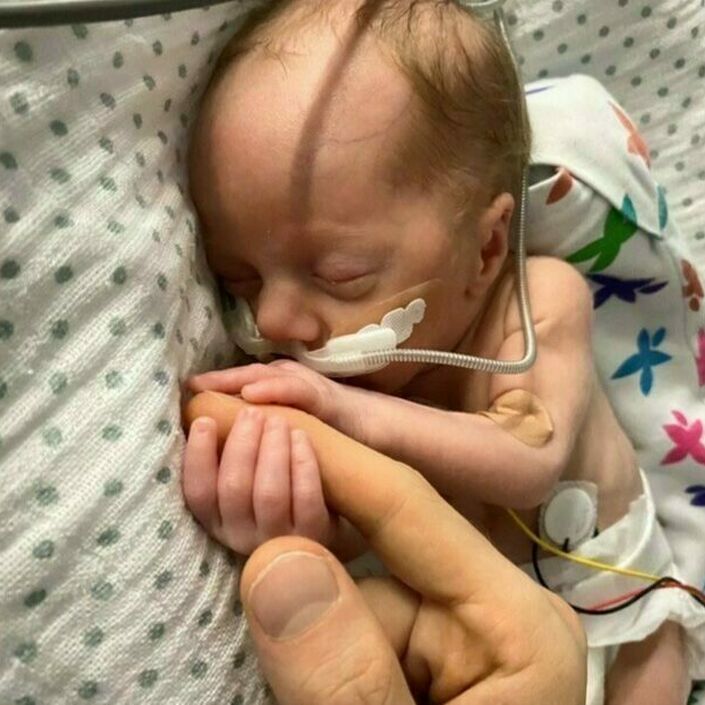
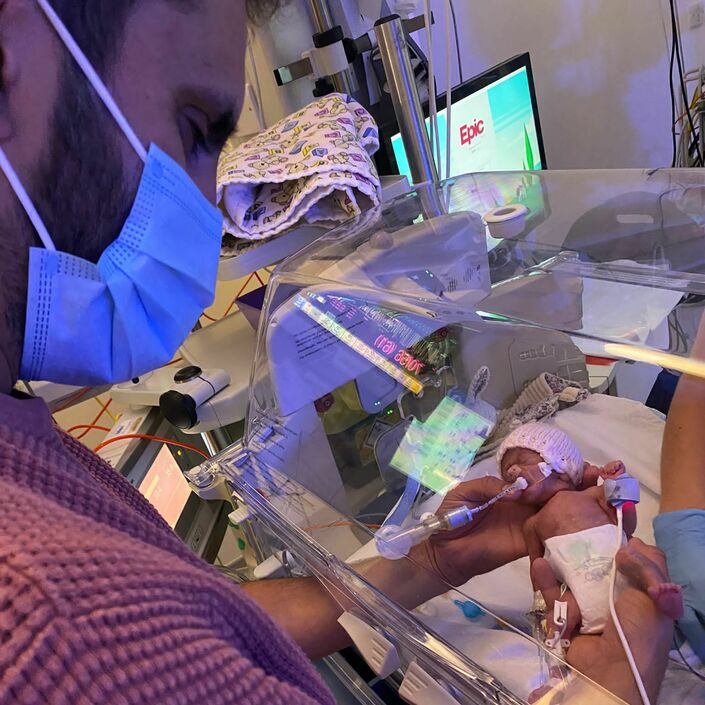
Zara was intubated and had wires and monitors attached everywhere, her eyelids were still fused shut, her little limbs just seemed so fragile and skinny. We always thought incubators looked small but compared to Zara, her incubator was cavernous. Five hours later, she was stabilised enough that we could both go to the NICU to see her.