My husband and I began the process of IVF over two years ago. We were lucky enough to get pregnant on our first attempt. We had the embryo transfer in March 2017 and had to wait ten days to take a pregnancy test. As you can imagine, we could hardly sleep as we waited to take the test. We were a whole mix of emotions – feeling anxious, excited and nervous all at once.
The test confirmed what we had dreamed of – I was pregnant! I couldn’t take it all in at first and had to do another test before I believed it. I then called my sister-in-law to triple check I was reading the results right.
A week later, we decided to pay for an early scan because I’d been having a horrific reaction to metoclopramide, an anti-sickness tablet that I was taking to help my severe vomiting (hyperemesis gravidarum).
As soon as the sonographer put the ultrasound on my stomach I yelled, “There’s two!” We were all very shocked – including the sonographer. It turned out the embryo was really high quality and split creating MCDA twins, which only happens in two per cent of cases.
MCDA twins share a single placenta with a single outer membrane and two inner membranes. We had our scheduled appointment with my IVF consultant at seven weeks and she said there was already a size difference between the babies. From that appointment on I was seen once a week during my first trimester to see if the size difference continued to show. There was talk of twin-to-twin transfusion syndrome (TTTS) but there was no confirmation of this.
A TTTS diagnosis is extremely worrying. It happens when there are blood vessels within and on the surface of a shared placenta which connects both twins. This causes the blood flow to become unbalanced, resulting in one twin (known as the donor) donating blood to the other twin. This results in the donor twin’s reduced growth and the recipient twin having too much blood which puts a strain on their heart.
At 12 weeks, I was referred to a foetal medicine consultant at my local hospital who scanned me and spoke to me about TTTS and its possible risks. I was told that if TTTS developed, I might have to have a laser ablation – a risky procedure that could put the twins’ lives in danger. At 16 weeks, the consultant said that she could not really see a bladder on the smaller twin and that there was too much amniotic fluid around the larger one. The news was not good – this is what the early stages of TTTS looks like.
The consultant said she would like another opinion before confirming the diagnosis. We were referred to St George’s Hospital where I was scanned twice a week to see if the bladder, amniotic fluid and blood flow were improving. Unfortunately, there was no improvement and at 20 weeks, TTTS was diagnosed.
My husband and I were taken into a room to discuss our options. We were told if I carried on the pregnancy without intervention I could lose both the babies. The other option was have a laser ablation which, if unsuccessful, could see me lose one or both the twins. The stats given to us for the success rates of the laser ablation were very low so we had to make the agonising decision of what to do next. We felt as if we had our children’s lives in our hands.

Together, we decided to seek out more medical advice. I frantically looked online for an expert in TTTS and came across the Harris Birthright Centre where Professor Kypros Nicolaides worked. I called his secretary and told her we had been given a few days to make our decision and she was able to book me in for an appointment the following day.
When we arrived at the appointment, I was scanned and the professor confirmed it was stage two TTTS. He said that the best thing to do to give either twin the chance of survival was to have the laser ablation that day. The procedure would be done on the donor twin because he had a smaller share of the placenta. The odds were not stacked in his favour but the ablation went as well as it could have. The Professor was pleased with the outcome and sent us home that evening.
From then on it was a waiting game to see if it had worked. I was constantly in and out of hospital and had a number of overnight stays. We were also scanned weekly by the foetal medicine team to see how things were going. Each week my smaller twin would gain around 25g. Each scan triggered a range of emotions – sometimes we had great news and other times it was bad. We were constantly told that the laser ablation had saved the bigger twin but there was no guarantee about the smaller one. As you can imagine, this was heart breaking to hear and not something that parents who are expecting twins necessarily consider.
We were aiming to make it to 32 weeks but at 29+5 weeks, a scan revealed that the bigger twin had increased amniotic fluids and the smaller twins dopplers were becoming absent. This meant that the TTTS was coming back.
“I am really sorry but we have to deliver,” the sonographer said. I wasn’t surprised by her decision but knew the risk it would entail. The smaller twin was thought to weigh 575g. My local hospital was only a Level 2 NICU so calls were made to find somewhere where the smaller twin could be cared for. After speaking with all the Level 3 hospitals in and around London, two cots were found at Queen Alexandra Hospital in Portsmouth.

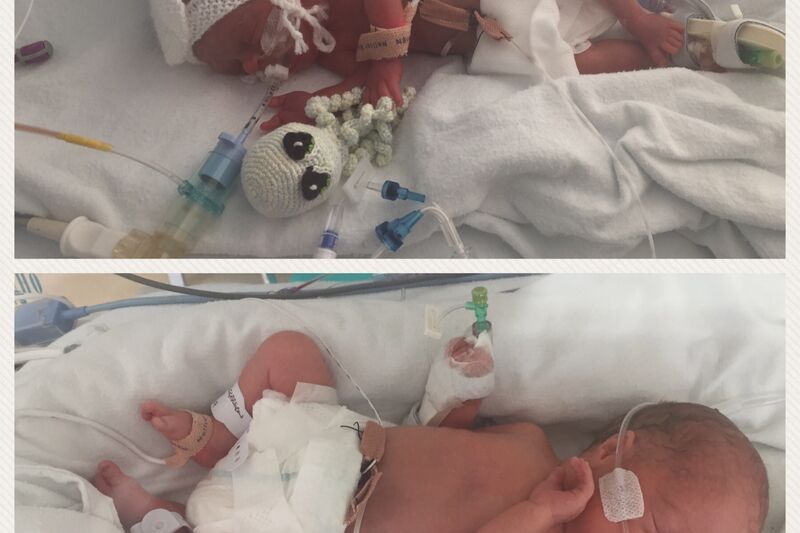
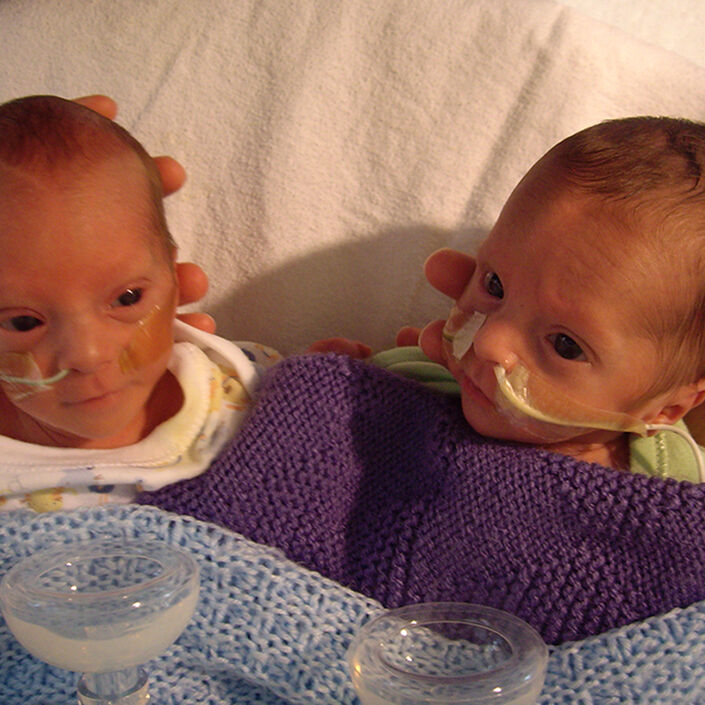
With a matter of urgency, I was blue lighted from Frimley Park to Portsmouth to deliver the boys by c-section that night. Unfortunately, further complications delayed the delivery until the following morning. On 15 September, our beautiful boy Teddy was born weighing 609g and a minute later our gorgeous Ronnie came into the world weighing 2lb 13oz. Two large teams were on hand to immediately work on our boys. After managing to settle the twins, they were transferred to NICU.
Ronnie’s NICU stay was 46 days and on the day of his discharge Teddy was transferred back to Frimley Park where he remained in NICU. We hoped that it wouldn’t be long before his discharge so that we would be reunited as a family once more. Finally, after 88 days we got to bring Teddy home. We were so excited for the boys to be back together again. We love watching them grow up together after such a long time apart.

If you have been affected by any of the issues mentioned in this post and would like support, view our online support pages.