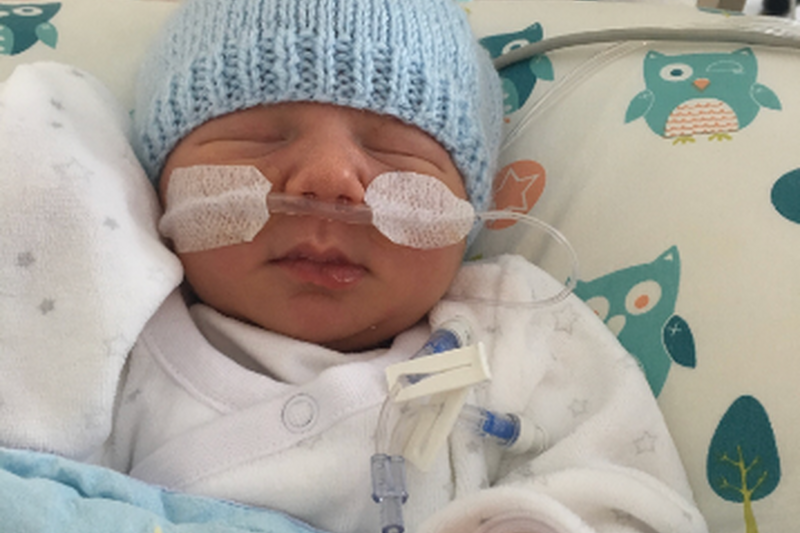
Our little boy was born at 40+3, weighing in at a standard 7 pounds 10 oz, after a very speedy but natural two-and-a-half-hour labour and delivery during the early hours. We were so thrilled to snuggle him - our second child, Caleb - and simply couldn’t wait to take him home, presumably later that day.
At around eight hours old, however, once settled on the postnatal ward, things took a turn for the worst. Caleb seemed uninterested in feeding and on reflection, became rather pale and grey in complexion. His eyes appeared to have a glazed over expression and I noticed that his breathing had become laboured. Looking at his chest, his ribs were pinching/sucking in when he was breathing.