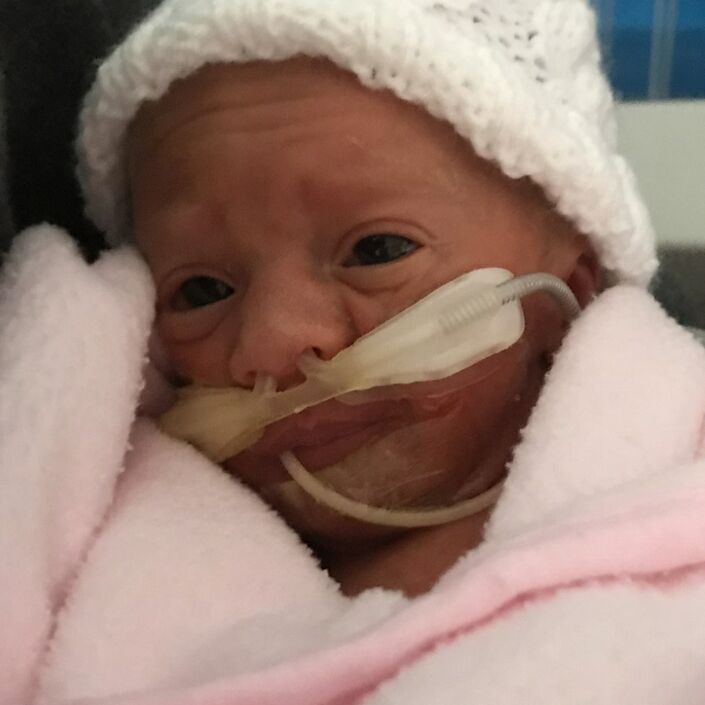
At 29 weeks pregnant, a scan showed high levels of resistance through the umbilical cord. It was confirmed that the placenta was slowly deteriorating, and our baby wasn’t growing as he should be. He was diagnosed with Intrauterine growth restriction (or IUGR - when a baby in the womb does not grow as expected). We were told to prepare for an early delivery likely to be by C-section. Our baby was too small, and my pregnancy had become a balancing act.
Nothing can prepare you for that kind of diagnosis. My body was supposed to be keeping our baby safe and helping him to grow, instead he was having to fight to get what he could.
At 32+1, in mid-December, after a week in hospital and a last-minute struggle to find a local neonatal cot, Joshua was delivered by urgent C-section. He weighed just 2lbs 13oz. The neonatal doctor bought him to me for a kiss before he was taken away to the NICU. Amazingly, he was breathing independently.
That was the start of our NICU journey. It was not how I’d expected our pregnancy to end. We didn’t have a bouncing bundle of joy that we took home 24 hours or so after delivery. Going in the lift from the post-natal ward to the NICU in the early days and seeing other families leaving the hospital with their new babies was really tough. I’d not had the huge bump of the third trimester that brings so much excitement as everyone gets ready for the new arrival. Or the water birth at 37+ weeks I’d hoped for.