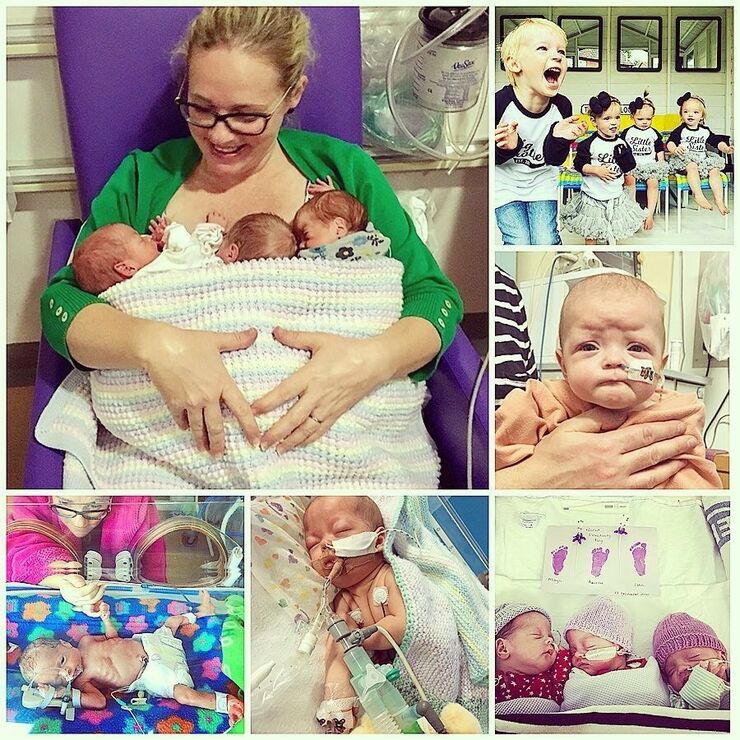
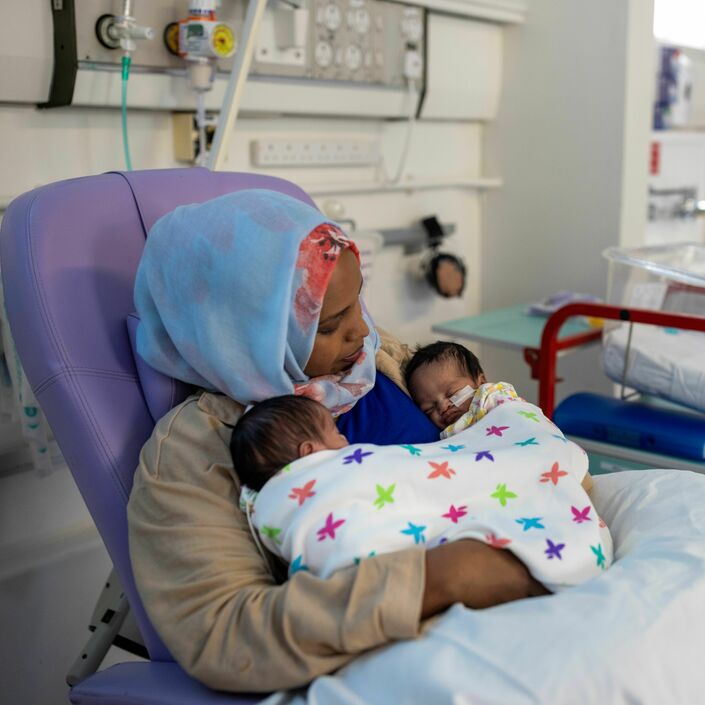
Following a traumatic arrival at 29 weeks gestation, my triplet girls Bertie, Etta and Amelie spent the first 11 weeks of their lives in hospital. They were the longest weeks of my life.
Outside of the hospital doors everyone else’s life continued. I felt locked in a vacuum of NICU and trauma but in my other life my son was at home and he needed me. So, every day I stopped at the ward exit teetering on the edge, questioning myself: “Can I leave yet? Can I do it? Can I leave my babies?”
In order to protect my sanity, I’d visualise an invisible force field drawing up around me to stop the hurt getting in and then I’d walk out of the door. If I didn’t use this invisible blanket to protect me from the hurt, then how could I have ever left my babies where they needed to be to get well?
There was still so much guilt. I’d worry about the long term impact of my invisible force field. Would it affect my bond with my daughters? I continued to use the protective force field to cope with the other areas of NICU life.
Things can change in an instant in NICU. On a daily basis you are reminded of this. I remember a day that started like any other. Bertie became very unwell and there was a dispute about what to do between the ward sister and the doctor on duty. The concern was that she was showing signs of sepsis. I stepped out of the dispute. I had to trust that the medical staff would get it right.
Later that day, as I fed Amelie, a doctor sat updating records on the ward computer. I watched as she jumped up towards Bertie and shouted for help. I sat there as medical staff surrounded my baby girl’s cot. Bertie had stopped breathing. I remember pulling up my invisible field around me. I looked straight ahead, I held Amelie close, and I tried to ignore the chaos around me. I couldn’t cope with my fear. I buried my head in the sand. I called it the ostrich effect.
Five weeks into the girls initial 11 weeks in hospital, I was diagnosed with Post Traumatic Stress Disorder. I received this diagnosis as a result of the life threatening birth trauma I had experienced. Unfortunately, in the year that followed the girls’ birth, we were to experience a series of significant health traumas that would leave me emotionally crippled by PTSD.
After their birth on 15 October, Bertie and Etta made it home for Christmas. On 28 December I brought Amelie home. I was overwhelmed with relief for my girls that they woke up in their home, not a ward. That my face was the first they saw every morning. I was relieved that now we could get on with our lives as a new family of six. That relief would be short-lived.
Within days of coming home, Amelie was back in intensive care in a medically induced coma fighting for her life. After three days in intensive care, Amelie was well enough to be transferred to our local hospital. As we arrived Bertie, who was also ill with paraflu taken by an emergency ambulance to a High Dependency Unit.
When both girls came home my PTSD was crippling. It was clear from the doctors’ response that if Amelie hadn’t been in my arms when she had stopped breathing that we’d have lost her. I was terrified to leave my babies alone. I was terrified that something awful would happen. I would walk into a room and brace myself for what I might find. That is the legacy of trauma; something terrible had already happened, so it could happen again.
My life became an overwhelming cycle of trying to keep my children safe. Every time we had a visitor I was braced with anxiety. I didn’t want anyone to touch them and possibly share their germs. It became easier to not have visitors and not to go out.
PTSD made me want to isolate myself and my family. I wanted everything to be perfect for the girls and didn’t want anyone to help with their care. This was mainly related to my fear of other people being near the girls in case they caught germs, but it was also due to my wanting to be their primary carer without interruption.