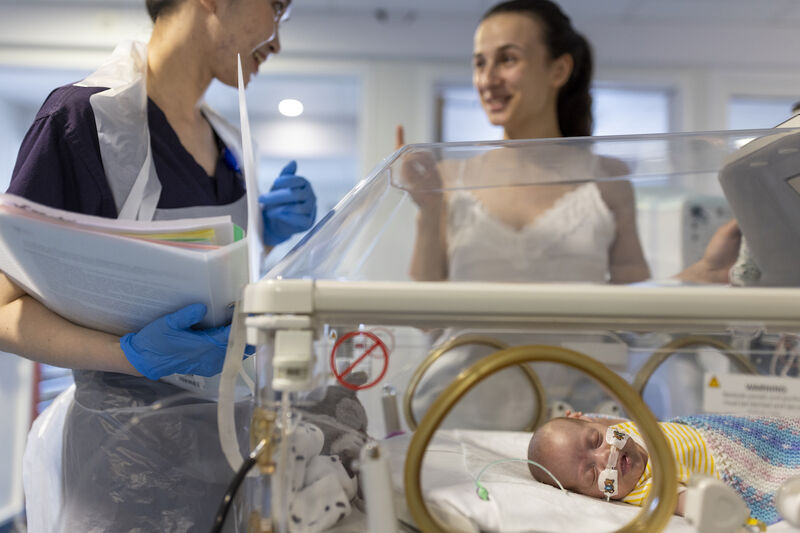
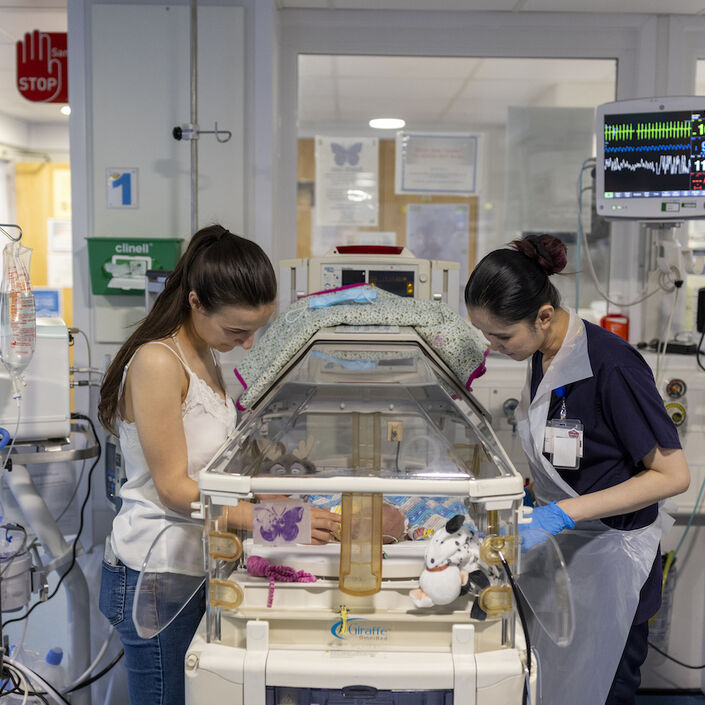
In focus groups held with members of our PAG, we learned about how they respond to communication, and how effective communication with healthcare professionals can improve their experience while on the neonatal unit.
Insight from our Parent Advisory Group
Parents said that communication was a driving factor in how comfortable and included they felt on the unit. Effective communication was also cited as the best way to make parents feel they are a central aspect of their baby’s care.
Below are some of the many key points raised in these focus groups that staff members should be aware of and respond to within the family-integrated care (FICare) environment.
Form of communication
- Parents noted concerns that arose when information about their baby was in their discharge notes but had not been communicated during the neonatal stay. This caused increased stress at discharge during an already stressful transition to home.
- Some parents said that question-and-answer techniques had limited effectiveness and can cause a lengthy delay in the transfer of information. Actual dialogues between families and medical staff were noted as the most effective form of communication.
- Some parents noted how communication about their baby’s prognosis can oftentimes feel very impersonal, such as the use of survivorship statistics. A more personal discussion about their baby and how it may affect their development would have been favoured and would have provided the family with a more tangible understanding of their baby’s future.
Timeliness of information
- Oftentimes, if parents were provided with information at the appropriate time and without unnecessary delay, difficult or sensitive news was easier to manage.
- Challenging moments for parents were examples such as when a baby is moved to another room without telling the parents in advance.
- Lapses in communication such as these can cause unnecessary worry and concern for parents if they are kept out of the loop.
- A quick phone call makes all the difference for parents.
Tailoring of information
- Some parents would prefer to discuss their baby using more medical terminology, whereas others would prefer a more simplified version.
- It is important that staff are aware of parents’ communication preferences and tailor their language to involve families as much as they would like.
Inter-staff communication
- Several parents mentioned the importance of inter-staff communication and how this impacted communication with parents.
- If staff are unaware of what other staff members had told parents, repetition or, conversely, missed communication can occur.
How can this be applied to FICare?
In the context of FICare, there is a lot that can be done in response to parents’ communication needs and preferences. Processes should be in place to ensure that parents’ communication preferences are identified, documented and referred to by all relevant staff throughout the neonatal journey.
In doing so, parents and families can experience consistent support and information while on the unit which can have a significant impact on their well-being. By tailoring communication appropriately, neonatal staff can ensure that parents are receiving the information they want and in the most appropriate manner for them.
In addition to accommodating for parents’ preferences, it is a crucial part of FICare culture that staff understand the importance of communication and how to effectively communicate with parents in a healthcare setting. This may require training to ensure consistency among staff, and processes should help guide staff members to carry this out in practice.
There is also scope for units to avoid reliance on question-and-answer techniques for communication between parents and medical staff, and efforts should be made to allow for face-to-face dialogue or phone calls.